Search
Results for 'what is an'
Clear-
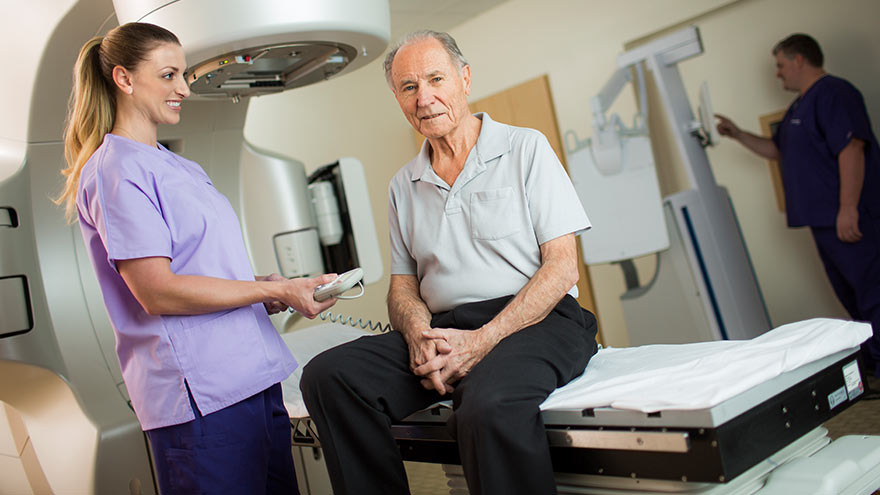
What Is the Importance of Having an Institute for Cancer?
What is an institute for cancer — and why does it matter that we have one right here in Reno? Here, a radiation oncologist answers those questions and more. Sadly, our community health needs assessment shows cancer is the second leading cause of death in Washoe County. But many residents may not know there is an institute for cancer right here in Reno that can care for you or your loved one after diagnosis. Dr. Michael Hardacre, a radiation oncologist with Renown Institute for Cancer is here with more. What is an institute for cancer? The way I like to think of it: An Institute has healthcare providers highly trained in patient-centered care. For example, when you have cancer, many times you’ll see a lot of doctors. A program brings those doctors together — so you really have one team working together. An Institute takes that one step further. Say there are other needs beyond the doctor’s office such as nurse navigators, dietitians, physical therapists to help you get on track, etc. An Institute really proactively thinks of the need of the cancer patient. It then makes sure all those things are available to them throughout their treatment. The term “institute for cancer” identifies a cancer program that is comprehensive and multidisciplinary in nature. For Renown, that means that we have the specialists in medical oncology, surgical oncology and radiation oncology working together with other specialists to assure that a patient has coordinated care throughout the entire treatment course of cancer care. Together with cancer prevention and diagnostics, genetic assessment, supportive care, clinical trials, and cancer survivorship, the institute for cancer provides care for the community, families and patients along the entire spectrum of cancer care. What types of cancer do you treat? We’re fortunate to be able to provide cancer treatments for all types of cancers, and we’re one of the major referral centers for northern Nevada. Most commonly, just like much of the country, lung cancer, prostate cancer and breast cancer are the most frequent we see. Our care spans brain, to neck cancer and everything in between. As an accredited comprehensive community cancer program, Renown Health provides services for all cancer types. The highest volume cancers treated at Renown are breast, colorectal, lung, genitourinary, blood and gynecologic cancers. Most treatments can be done right here in Reno, but when there are specialty needs such as stem cell or bone marrow transplantation, we partner with quaternary centers, like Stanford, to assure a smooth transition of care both to and from the quaternary center. What kinds of care and treatments are offered? We offer a wide range of comprehensive care. We treat the cancer itself — surgical, radiation oncology, medical oncology in the form of chemotherapy or pills. Also addressed: dietary needs, physical therapy and navigation through this whole process. People may be surprised by the scope and scale of the Renown Institute for Cancer. For instance, our Radiation Center has the latest technologies to treat cancers. This includes the Linear Accelerators, which are machines with treatment planning software tools. In addition to the traditional external radiation treatments provided in most centers, Renown performs specialty treatments using High-Dose Brachytherapy, a treatment with an active radiation “source” and in Brain Stereotactic Radiosurgery, assuring that patients can stay right here in northern Nevada — close to home. What does that mean for the quality of care? I think it’s always great in any environment to have external people come into your program and not only share what’s happening nationally and what we could do better, but also to validate “are you doing things at the highest level you can?” That accreditation process is just one way to give us that seal of approval. We’re lucky enough this year to get the gold award by the American College of Surgeons — its highest honor. We were honored to receive it. Why is important that you’re an accredited institute? Accreditation assures our community that quality is a top priority for us. Each of the accrediting bodies has a set of standards that identify service and quality standards. Renown Institute for Cancer has the following accreditations: American College of Surgeons’ Commission on Cancer: Full Cancer Program accreditation, standards address issues from cancer prevention/diagnosis to treatment to survivorship and/or end-of-life. Renown received the Gold Level Accreditation in 2018, the highest level of accreditation possible; American College of Surgeons’ National Accreditation Program for Breast Centers: Full Breast Center/Program accreditation, standards address issues from breast cancer prevention/diagnosis to treatment to survivorship and/or end-of-life; American College of Radiology – Radiation Therapy: Full Radiation Oncology accreditation for radiation equipment, treatment planning, treatment and treatment follow-up; and American College of Radiology – Mammography Services.
Read More About What Is the Importance of Having an Institute for Cancer?
-
What Is the Role of a Child Life Specialist?
What is the role of the child life specialist? Here are common questions and answers about how these special individuals give both parents and kids peace of mind. Let’s face it: A hospital can be an intimidating place for just about anyone. But add in being a small human with very little worldly experience — aka a child — and it’s easy to imagine how overwhelming a hospital visit can be. Enter the role of the child life specialist. Liz Winkler, a child life specialist with Renown Children’s Hospital, explains how a Renown program puts young patients and their families at ease. What does a child life specialist do? Child life specialists help young patients develop ways to cope with the anxiety, fear and separation that often accompany the hospital experience. They give special consideration to each child’s family, culture and stage of development. As professionals trained to work with children in medical settings, specialists hold a bachelor’s or master’s degree in the areas of child life, child development and special education or recreational therapy. Our child life specialists are also professionally certified and affiliated with the national Child Life Council. Child life specialists also offer tours of Renown Children’s Hospital for families whose children are scheduled to have surgery. Child life supports children and families by: Helping children cope with anxiety, fear, separation and adjustment Making doctors, needles and tests a little less scary Providing art, music and pet therapy Organizing activities Addressing your concerns Telling you what to expect Creating a therapeutic and medical plan Offering a hand to hold What else is available at the Children’s Hospital that helps ease some of the stress of a hospital visit? Whether it’s seeing a pediatrician, getting a sports physical or looking for advice, our care is centered on supporting and nurturing patients and families at our many locations. We have kid-friendly environments to help ease some of the stress of a hospital visit. These include colorful exam rooms, kid-friendly waiting and common areas, and medical equipment designed especially for children. Our children’s ER is open 24 hours a day, seven days a week. So parents and caregivers have access to emergency care tailored to little ones — anytime, day or night. We have several pediatric specialists on the Renown team in areas including diabetes, emergency medicine, neurology, pulmonology, blood diseases and cancer. How can parents start to ease their children’s mind when they know a hospital visit is in the future? As with many things in life, good preparation can help kids feel less anxious about the experience and even get through recovery faster. It’s important to provide information at your child’s level of understanding, while correcting any misunderstandings, and helping to eliminate fears and feelings of guilt. If you’re anxious and nervous, your child may reflect these feelings and behaviors. So make sure you educate yourself, feel comfortable with the process, and get your questions answered.
Read More About What Is the Role of a Child Life Specialist?
-
What is Polycystic Ovary Syndrome (PCOS)?
Dr. Carilyn Hoffman with Renown's Women's Health explains the symptoms, causes and treatments of Polycystic Ovary Syndrome (PCOS) (also referred to as Polycystic Ovarian Disease (PCOD)), a prevalent condition among women of reproductive age that influences hormonal balance, metabolism and fertility. Make an appointment with Renown Women's Health Click here to schedule Call to schedule: 775-982-5000 PCOS Defined PCOS is a constellation of symptoms characterized by two of the three criteria: multiple small cysts on the ovaries visible via ultrasound, irregular periods and signs of hyperandrogenism. Other symptoms include infertility, insulin resistance, and increased risk of cardiovascular disease. Symptoms of PCOS The symptoms of PCOS can vary from woman to woman, but some of the most common include: Irregular menstrual cycles: This is often one of the first signs of PCOS. Women may experience fewer than nine periods a year, more than 35 days between periods, frequent spotting, and/or abnormally heavy periods. Excess androgen levels: High levels of male hormones may result in physical signs such as excess facial and body hair (hirsutism), severe acne and male-pattern baldness. Polycystic ovaries: Enlarged ovaries containing numerous small cysts can be detected via ultrasound. Causes and Risk Factors The exact cause of PCOS is unknown, but several factors may play a role: Genetic predisposition: A family history of PCOS increases the risk. Insulin resistance: High insulin levels might increase androgen production, causing difficulty with ovulation. Obesity: Women with elevated BMI’s are more likely to have PCOS, although 20% of women with PCOS are not obese. Diagnosis and Treatment Dr. Hoffman outlines that diagnosing PCOS requires a medical history review, a physical exam, blood work and an ultrasound to evaluate the ovaries. Treatment options can range from lifestyle modifications, like diet and exercise and weight loss, to medications for menstrual regulation, fertility assistance, and rarely surgery. Lifestyle Changes A healthy lifestyle is a cornerstone of managing PCOS. Regular exercise, a nutritious diet, and weight management can help reduce symptoms and the risk of long-term health issues. In overweight patients, weight loss as little as 5% has been shown to improve symptoms of PCOS. Medication Medications may include hormonal contraceptives to regulate menstrual cycles, anti-androgens to reduce hair growth and acne, and Metformin to address insulin resistance. Fertility Treatment For women with PCOS who are trying to conceive, ovulation induction with clomiphene or letrozole is sometimes necessary. Sometimes a referral to a reproductive endocrinologist and infertility specialist is needed for more advanced technologies like IVF. Health Implications PCOS is not just about cystic ovaries or irregular periods; it can have profound implications on a woman's overall health. Women with PCOS are at an increased risk for several conditions, including type 2 diabetes, high blood pressure, heart disease, and endometrial cancer.
-
What it Means to be a Level II Trauma Center
When the sudden need for emergency or critical care arises, the level of a trauma center is an important designation that helps explain the types of resources available. Renown Regional Medical Center is proud to be the only Level II Trauma Center in our region, which is a critical service to provide. We spoke with Bret Frey, MD, an emergency care physician, to discuss what this means for our community. Requirements for Designation as a Level II Trauma Center To be a designated Level II Trauma Center, a hospital must have 24-hour immediate coverage by general surgeons and multiple specialties, such as orthopedic surgery, neurosurgery, emergency medicine and more. In addition, this hospital must provide trauma prevention and ongoing education for its teams and incorporate a comprehensive quality assessment program. “What it means for this community is nothing short of amazing,” said Dr. Frey, who explained that Renown has over 20 specialty physicians on-call and ready to provide trauma care. According to Dr. Frey, many communities of the same or larger size have fewer specialists ready and available to provide this level of care. Renown Regional Medical Center is located near downtown Reno. The Emergency Department has several helipads and ambulance banks to intake patients requiring emergency care. Patients can also receive emergency walk-in care. On the same campus is Renown Children’s Hospital, which is home to the only pediatric Emergency Room dedicated solely to pediatric patients. Emergency and trauma care is just one area in which Renown Health is the regional leader. When patients or families choose Renown during an emergency, they will have access to all the resources provided through the entire health network. This means access to the many specialists available to consult on different conditions or care situations, inpatient care if needed, referrals to other areas of the network and medications to go. “I’m very happy and proud to be a part of building something very special in this community,” said Frey.
Read More About What it Means to be a Level II Trauma Center
-
What Does It Mean to Participate in a Clinical Trial?
Participating in a clinical trial is voluntary and a personal choice. Clinical trials are research studies that involve people and are an important part of patient care. What is a clinical trial? Clinical trials are research studies that involve people, and they are an important part of patient care. There are several different types of clinical trials; some are designed to understand trends in a disease or identify better ways to diagnose a condition, while others determine if a new treatment is safe and works when treating, improving or preventing a health condition. There are over 400,000 clinical trials currently being conducted in the United States, and even more across the world. This includes health conditions such as heart failure, cancer, Parkinson’s Disease, respiratory conditions like COPD, common infections, cystic fibrosis, and many more. Clinical trials lead the healthcare industry to new discoveries that contribute to reliable and exact care, improving healthcare quality and saving lives. Clinical trials are conducted by a team of researchers, including doctors, pharmacists and clinical research coordinators. These research teams are highly skilled in their specialty areas, often providing traditional patient care and seeing research patients in the same day. These teams are responsible for making sure the clinical trial is completed correctly, and their patients are their top priority. Why should I consider participating in a clinical trial? Participating in a clinical trial is voluntary and a personal choice. There are many reasons why patients decide to get involved in clinical research. While many clinical trials are designed for patients who have a certain health condition, many studies also ask healthy volunteers to contribute in order to compare health outcomes. Clinical trials are also for patients at all different stages of their diagnosis. Depending on the specific study, the patient may receive access to a new cutting-edge treatment before it is widely available. When patients join a clinical trial, the research team becomes a health partner dedicated to their health and well-being. When patients join a clinical trial, they make an informed decision in their healthcare by weighing all available options in addition to routine treatments. Research participants know that they are contributing meaningfully and helping other patients like them. Where can I find more information about clinical trials at Renown Health? Renown Health’s mission is to make a genuine difference in the health and well-being of the communities we serve. Renown’s clinical trial portfolio offers leading care options to patients in northern Nevada, close to home, in a variety of specialties. Contact the Renown Clinical Research Office for more information on clinical trials available to you!
Read More About What Does It Mean to Participate in a Clinical Trial?
-
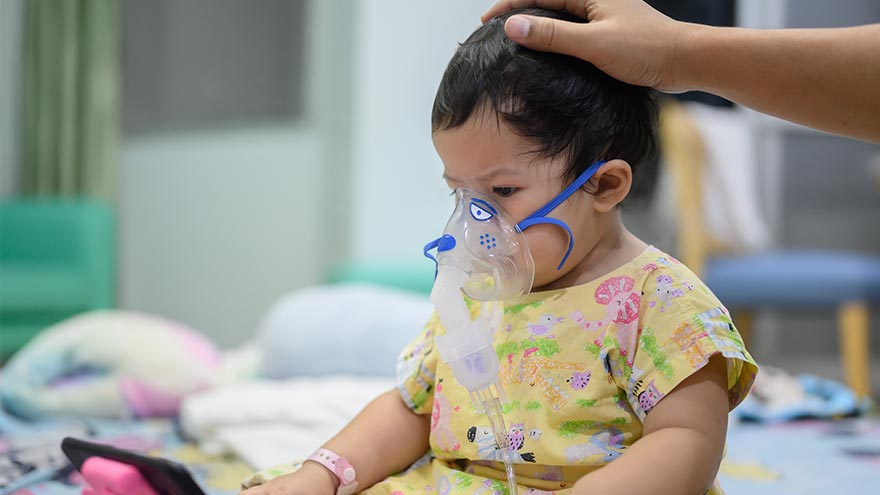
What You Need to Know About RSV
Respiratory syncytial virus, also known as RSV, is a common respiratory virus that impacts the lungs and breathing pathways. The virus can be dangerous for infants and young children and is also concerning for older adults. While most older kids and adults only experience cold-like systems and recover in a week or two, an estimated 58,000-80,000 children younger than 5 years old are hospitalized due to RSV each year, and in 2022 healthcare organizations across the country are experiencing higher infection rates than in years past. "We are experiencing a strong RSV season and do not expect it to go away anytime soon," said Dr. Kris Wilson, Division Chief of Renown Children's Primary Care. "Infants who are infected with RSV almost always show symptoms of runny noses and cough. Call your healthcare provider immediately if your child is having difficulty breathing, is not drinking enough fluids, or is experiencing any worsening of these symptoms.” Symptoms of RSV: Runny nose Decrease in appetite/inability to drink Dry diapers, an indication of dehydration Cough, which may progress to wheezing or difficulty breathing Irritability (most common in very young infants) Decreased activity (most common in very young infants) Decreased appetite (most common in very young infants) Apnea, pauses in breathing for more than 10 seconds (most common in very young infants) What to do if you think your child has RSV: Call your pediatrician! If you suspect your child might have RSV, consulting their healthcare provider is the best first line of defense. From here they will help you build an appropriate treatment plan for child. Keep in mind that many pediatrician offices offer 24/7 call lines. If your child is experiencing retracted breathing (when the area between the ribs and in the neck sinks in when a person attempts to inhale), dehydration (not drinking and decrease in wet diapers) or apnea (pauses in breathing for more than 10 seconds) please call 911 or go to the closest emergency room.
-
What's Special About Nursing at Renown Health
At Renown Health, we live by a core set of values. We are caring and compassionate. We demonstrate respect and integrity. We build relationships and collaborate with patients, families, clinicians and communities. We strive for excellence in all we do. Those values extend beyond patient care to the way we support our employees. We have worked hard to create an environment that empowers each person to learn, grow and thrive. Here are just a few examples of the ways we do that: Establishing a mentorship and leadership development program that provides insight, expertise and learning opportunities. Forming employee committees that improve health and well-being both at work and in our community that complement Renown’s work-life balance programs. Recognizing and rewarding team members for living our values. Providing paid time each quarter to support employee volunteerism and giving back to our community. Offering a variety of education programs, including tuition reimbursement, student loan repayment and a professional advancement bonus program, to help employees achieve their higher education goals. Hosting the largest Graduate Nurse Residency program in the state, which is also one of the largest in the nation. We strive to inspire, educate and help nurses shine, and in return, we know they will make a positive impact on the lives of their coworkers and the people we serve.
Read More About What's Special About Nursing at Renown Health
-
What to do if you Experience a Summer Burn
As families spend more time outdoors to enjoy the summer temperatures, it's important to be aware of potential hazards that can lead to burns – be it sunburns, burns sustained while grilling or navigating the hot surfaces often found around pool decks and parks. All these burn types are not only painful but can also cause severe damage to the skin and require immediate medical attention. Ross Albright, MD, an emergency care physician, explores effective preventive measures to avoid burns during the summer and discusses when it's essential to seek medical care. Stay Sun Safe While soaking up the sun is a favorite summer pastime for many, it's important to protect your skin from harmful ultraviolet (UV) rays. Sunburns not only damage the skin but also increase the risk of more severe burns. Follow these tips for staying safe in the sun: Apply broad-spectrum sunscreen with a minimum SPF of 30 before heading outdoors and reapply every two hours. Seek shade during peak hours of sun intensity, typically between 10 a.m. and 4 p.m. Wear protective clothing, such as wide-brimmed hats, sunglasses and lightweight, long-sleeved garments. Fire and Hot Object Safety Summer is full of fun outdoor activities like BBQs, campfires and fireworks, all of which can pose a fire hazard if not handled carefully. To prevent burns caused by fires: Maintain a safe distance from open flames and grills and always use oven mitts or potholders when handling hot objects. Keep a fire extinguisher and a first aid kit readily available. Keep children away from hot objects and fireworks and educate them about the dangers of touching or playing with them. Hot Surface Safety Asphalt, metal slides and surfaces around the pool retain heat and are likely to be significantly hotter than other materials such as a wooden picnic table to grassy pathway (these can still be hot too!). So, it's crucial to be cautious around these materials to prevent burns: Use caution when near hot surfaces surrounding water sources, such as pool decks or metal slides. Always wear shoes when walking on hot surfaces such as asphalt, concrete and even sand. Ensure that playground equipment such as slides and swings are cool to the touch before your kiddos start climbing around. Recognizing Severity of Burns and Seeking Care Despite our best efforts, burns can still occur. It's essential to know when a burn requires medical attention: First-degree burns, characterized by redness, pain and minor swelling, can typically be treated at home with cool water and over-the-counter pain relievers such as ibuprofen (Advil or Motrin) or acetaminophen (Tylenol). Second-degree burns, which may cause blistering and more intense pain, should be evaluated by a healthcare professional. Third-degree burns, indicated by charring or blackened skin, deep tissue damage or burns that cover a large area, require immediate emergency care. Preventing burns during the summer is paramount to enjoying a safe and enjoyable season. By following these tips, you can significantly reduce the risk of burns and ensure prompt medical attention when necessary. Stay informed, stay safe and have a burn-free summer! If you or someone you know experiences a burn, it's important to seek immediate medical care.
-
You're Ready to Start a Family! Now What?
Deciding you’re ready to start a family is a big decision for any couple. So once you’ve decided – what are the next steps for both moms and dads-to-be? And what should you know if you’re struggling to conceive? Dr. Myron Bethel, OB/GYN with Renown Women’s Health, offers key insights about fertility. What’s the first thing couples should do when they decide to start a family? For the mom-to-be, it’s important to meet with your obstetrician before you get pregnant. This appointment gives you an opportunity to discuss your family medical history, any past or current health problems, immunization history, medications you’re taking and any issues with previous pregnancies. Your doctor can also provide helpful tips to ensure your body is ready for a healthy pregnancy and help guide you on how to monitor your period, basal resting body temperature and other important factors to help you get pregnant more quickly. How can couples who are trying to get pregnant make sure they’re healthy to conceive? Of course it’s important to maintain a healthy lifestyle all the time, but it’s especially important if you’re trying to get pregnant. There’s no magic pill or single food, but women should start focusing on nutrients they’ll need during pregnancy. Before trying to conceive, start taking folate and folic acid to help prevent birth defects. You can get good sources of these nutrients from cereal, spinach, beans, asparagus, oranges and peanuts. Lifestyle changes can also help improve fertility. For both men and women, extra weight can reduce fertility. Both sexes can increase their chances of conception by not smoking, not drinking alcohol and exercising regularly. And for men specifically, take a daily vitamin containing zinc and selenium to support healthy sperm. What is the average timeline for conception, and what do you suggest for couples who may be struggling to conceive and start a family? First, remember getting pregnant can take longer than you expect. Do not to get stressed out about it or place blame. Seventy percent of couples conceive within six months and 85 percent within one year of trying to get pregnant. To help improve your chances of pregnancy, monitor your ovulation closely. You can do this by tracking your period, watching your body closely and logging symptoms, logging your basal body temperature or using ovulation kits. If you still aren’t sure when you’re ovulating, try to have sex every other day to improve your chances of conception. If you’ve been trying for nine months to a year, you can talk to your OB about options and discuss meeting with a fertility specialist.
-
Life after Lymphedema Diagnosis: What to Expect
Managing lymphedema effectively is essential for enhancing the quality of life for individuals affected by this condition. Katherine Bunker, a Physical Therapist and Certified Lymphedema Therapist (PT, DPT, CLT) at Renown, has expertise in this area and her insights offer valuable strategies for managing lymphedema. Lymphedema is a chronic condition characterized by swelling in one or more limbs due to a blockage in the lymphatic system. This condition can result from cancer treatments, surgery, infection, or can sometimes be congenital. While it can be challenging to live with lymphedema, understanding the condition and adopting specific lifestyle changes and strategies can significantly improve the quality of life. Understanding Lymphedema Educating yourself about lymphedema is crucial. Understanding the causes, symptoms, and potential complications can provide you with the tools to manage the condition proactively. Lymphedema can lead to discomfort, decreased mobility, and in severe cases, infections such as cellulitis. Therefore, recognizing the early signs and knowing when to seek medical advice is essential. Medical Management Consulting with healthcare professionals who specialize in lymphedema is critical. A physiotherapist or occupational therapist trained in lymphedema management can tailor a treatment plan for you that can include the following: Compression Therapy - Wearing prescribed compression garments can help move the lymph fluid and reduce swelling. It’s essential to get fitted by a professional and understand how to use these garments correctly. Manual Lymphatic Drainage (MLD) a gentle massage technique that encourages the movement of lymph fluid out of the affected limb. It’s typically performed by a trained therapist but ask about self-massage techniques you can do at home.
Read More About Life after Lymphedema Diagnosis: What to Expect
-
MD, APRN or PA: What's the Difference
Having a primary care provider is important and some health insurance plans even require you to select one. But does that provider need to be a doctor (MD)? The good news is your primary care provider doesn’t need to be an MD. They can be an advanced nurse practitioner (APRN) or physician assistant (PA). We’re here to explain the differences between MDs, APRNs and PAs. Have you ever called Renown Health to schedule an appointment with your doctor and the Contact Center offered you an earlier appointment with an APRN or PA? Did you wonder why? Perhaps you even declined because you were concerned about the continuity of your care, or wondered about the qualifications of the other practitioners who aren’t doctors. We’re here to answer your important questions about primary care providers and the different types. Why would I want to see anyone other than a doctor? In order to keep up with demand for primary care services and provide the highest quality care possible, Renown created care teams. This means our doctors, APRNs and PAs all work hand-in-hand to manage your health with the benefit of their combined expertise. This team approach provides you with more flexible scheduling options to see anyone on the care team, all with the same continuity of care. How qualified are APRNs and PAs to treat patients? APRNs and PAs are highly educated in medicine with a minimum of a Master of Science degree and at least six years post-high school education. Some APRNs even have doctorate degrees. Similar to doctors, both positions have a minimum number of required clinic hours and participate in continued education. Both APRNs and Pas are just as qualified as doctors (MDs and DOs) to conduct physical exams, diagnose and treat illnesses, order and interpret tests, write prescriptions and even deliver babies. There are some instances where you need a doctor, including specialized treatment of complicated or high risk conditions or surgery. Your APRN or PA will refer you to a doctor in those instances. You don’t need to worry about whom to see when – your care team will guide you based on your medical needs. If I see an APRN or PA, will my doctor know about my visit? Absolutely. The care team system ensures that everyone on your care team is aware of the details of your visit, regardless of who you’re seeing. Everything is clearly documented in your medical record so there are no gaps in care between visits. Can an APRN or PA be my primary care provider? Definitely. APRNs and PAs make excellent primary care providers and can be established with your insurance company. Learn more about the differences between doctors, APRNs, PAs and more with this handy infographic. Schedule A Doctor Visit | 775-982-5000 Renown Medical Group primary care providers provide annual exams by appointment. Our providers coordinate each patient’s medical care including checkups, immunizations, referrals to specialists, lab work, X-ray & imaging and hospital admissions. Request an Appointment
-
Preventing Spinal Cord Injuries: What to Know
If you're not taking safety precautions during mountain sports, you could be at risk for a spinal cord injury. Dr. Benjamin Pence of Renown Rehabilitation Hospital explains the best way to prevent this serious injury. Mountain sports are a big part of the winter season here in our area, but if you’re not practicing all the proper safety techniques, you could end up with a serious spinal cord injury. Benjamin Pence, MD, Renown Rehabilitation Hospital, is here to offer tips to prevent this serious injury while you’re out enjoying what the Truckee Meadows has to offer. What is the spinal cord? The spine stretches from the base of your skull to the coccyx (commonly referred to as the tailbone). Your spine is made up of 24 vertebrae—seven cervical, which are in your neck, 12 thoracic, which are in your chest, and five lumbar, which are in your lower back. There are ligaments and muscles attached to each vertebra. These facilitate back movement and protect the bones from damage. There is cartilage between each vertebra which acts as a shock absorber for your spine. Finally, the spinal cord is a long, thin, tubular bundle of the nervous tissue and support cells that is enclosed in the spinal canal and send signals from the brain to everything from your arm and leg muscles to bowel and bladder function. The brain and spinal cord together make up the central nervous system.
Read More About Preventing Spinal Cord Injuries: What to Know





.jpg?rev=f89fdc95b1824f868e98988928b0a6bb)