Search
Results for 'doctors'
Clear-
Here's How to Commemorate National Healthcare Decision Day
National Healthcare Decision Day is forthcoming. Here’s an easy and free way to commemorate the occasion: openly discussing how we want to be cared for at the end of our lives. Join Renown Health’s experts at a workshop about making decisions about an advance directive. Among the random national holidays, this one has significance: April 16 is National Healthcare Decision Day. And experts agree that the best time to discuss your views about end-of-life care and to learn what choices are available is before a life-limiting illness or crisis occurs. By preparing in advance, you can help reduce the doubt and anxiety related to decision making for your family if you cannot speak for yourself. “Completing your advance directive is a gift you give your family,” says Mary-Ann Brown, RN, MSN, director of Palliative Care. “The stress associated with these difficult decisions is decreased if everyone knows what is important to you and what you want the end of life.” What Are Advance Directives? An advance directive is a document that states your choices about medical treatment and names another person to make medical decisions on your behalf if you are unable to. This document allows you to make legally valid decisions about future medical care. Find more information about advance directives and the form online. The Conversation The first step in completing an Advance Directive is to think about what’s important to you and talk to your loved ones. The Conversation Project provides helpful tools to guide you and your family through this challenging topic. Getting this information together will help you fill out and complete your advance directives. Some things to consider and discuss with your family include: When you think about the last phase of your life, what’s most important to you? Who do you want involved in your care? Who should make decisions on your behalf if you’re not able to? Where do you want or not want to receive care? Are there specific treatments you would or would not want? Complete Your Advance Directive Planning In order to complete an advance directive, you will need either two witnesses or a notary to sign the form. Be sure to note restrictions on the witness process. When an advance directive is complete, you should keep the original. Copies should be given to your agent named in the form, your family, your doctor(s) and the location that you receive care. Renown Health offers four advance directive workshops every month to cover the details of filling out this document. A healthcare team is available to answer questions and work through the process with you. A notary is also present to finalize the process, which means you can complete your advanced directives during this workshop. Find the workshop by calling 775-982-RSVP for more information. Advance Care Planning Workshop April 17, 1-2:30 p.m. | Free Join Renown Health’s experts for a workshop about making decisions regarding end-of-life care. You will learn how to fill out an advance directive, receive one-on-one assistance and have your documents signed by a notary. Workshops are typically held several times each month. To RSVP, call 775-982-7787
Read More About Here's How to Commemorate National Healthcare Decision Day
-
3 Reasons to Choose a Senior Care Plus Health Plan
Senior Care Plus was Nevada’s first Medicare Advantage Plan and is still providing healthcare coverage to qualifying members in Washoe, Carson City, Clark & Nye Counties. Senior Care Plus is administered by Hometown Health, the insurance division of Renown Health. That relationship means Senior Care Plus is the only Medicare Advantage Plan supported and accepted at Renown. This preferred access to Renown is a great benefit for northern Nevadans. When it comes to healthcare coverage, there are three key factors to keep in mind. Here’s why a Senior Care Plus Medicare Advantage Plan is your best choice. 1. Cost Cost matters when searching for the right insurance plan. Of the four Senior Care Plus plans available to residents of Washoe County and Carson City, three offer a zero-dollar monthly premium and all of them offer zero-dollar primary care office visits. That means no out-of-pocket costs for you. Additionally, all Senior Care Plus plans have an annual out-of-pocket maximum. This means when you reach this amount, that’s all you will pay. Senior Care Plus pays all other covered medical benefits for the rest of the year. That’s the beauty of a Senior Care Plus Medicare Advantage Plan. 2. Size of Provider Network and Accessibility Although saving money is important, it’s more important to be able to see a doctor when and where you need to. Senior Care Plus members enjoy the most comprehensive healthcare provider network in the region. Thousands of providers, including many hard-to-find specialists, are in the Senior Care Plus network. Since Senior Care Plus is part of the Renown Health family, you get priority access to all that Renown has to offer, which you won’t find with any other Medicare Advantage Plan. 3. Coverage Medical coverage needs are personal and unique to every member. Understanding a plan’s benefits is essential when picking the best coverage for you. Of course, the important benefits you associate with a healthcare plan are included in all Senior Care Plus plans: urgent care visits, specialists’ visits, lab services, imaging — all with reasonable copays. What sets Senior Care Plus apart from the rest are the additional benefits for preventive health. For example, Senior Care Plus offers plans with a comprehensive dental benefit with first-dollar coverage, meaning you pay nothing until the benefit limit is reached. Senior Care Plus Medicare Advantage Plans also have a vision benefit allowing you to get a new pair of eyeglasses every year. In addition, these plans offer a fitness benefit, so you can join a local gym because Senior Care Plus wants to keep you healthy. Another interesting benefit is the over-the-counter benefit. If you choose the Renown Preferred Plan, you can select $50 worth of over-the-counter products such as: cold medicine, dental products, diabetic supplies, and digestive aides. Remember, that’s $50 worth of over-the-counter products four times per year. All on a plan that doesn’t cost a thing. Senior Care Plus Medicare Advantage Plans offer many added benefits tailored to Nevadans.
Read More About 3 Reasons to Choose a Senior Care Plus Health Plan
-
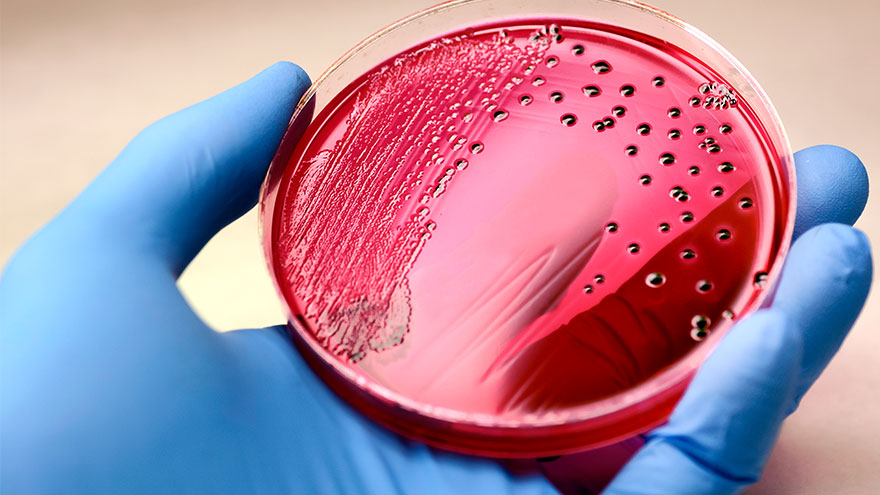
Sepsis: Causes & Symptoms
According to the Global Sepsis Alliance, 1 in 5 deaths worldwide are associated with sepsis. If not recognized early and treated promptly, sepsis is the final common pathway to death from most infectious diseases worldwide, including viruses such as COVID-19. We spoke with Jeremy Gonda, MD, a critical care physician from Renown Health’s Sepsis Committee to increase public awareness of this preventable medical emergency. What is sepsis? Sepsis is a response to infection—bacterial, viral or fungal—and can start anywhere in the body and spread into the bloodstream. The body is trying so hard to fight an infection that it begins releasing chemicals into the bloodstream that cause inflammation and the shutdown of multiple organ systems. “It carries a very poor prognosis in general unless you catch and treat it very early,” said Dr. Gonda. “Any infection can lead to sepsis. Typically your immune system takes care of the infection. It doesn’t progress, but in cases where the infection becomes severe, or the immune system doesn’t function properly, people can certainly die. So there’s, unfortunately, a very high mortality rate associated with sepsis.” According to the Centers for Disease Control and Prevention, each year at least 1.7 million adults in America develop sepsis. While you can recover from sepsis if caught early, many sepsis survivors suffer from long-term physical and psychological effects. What are the signs of sepsis? One way to spot sepsis is to use the acronym SEPSIS: S – Slurred speech and confusion E – Extreme shivering or muscle pain/fever P – Passing no urine all day S – Severe breathlessness I – “I feel like I might die” S – Skin mottled or discolored Keep in mind that sepsis symptoms can vary depending on where the infection starts. “Patients may experience urinary burning if they have a urinary tract infection or a cough and shortness of breath if they have pneumonia first,” said Dr. Gonda. “However, often symptoms are more generalized or subtle such as fevers, confusion and malaise.” How do you develop sepsis? When germs enter your body, they can cause an infection. If you don’t stop that infection, it can cause sepsis. Areas of infection that more commonly result in sepsis include: Lungs, such as pneumonia Kidney, bladder and other parts of the urinary system Digestive system Bloodstream (bacteremia) Catheter sites Wounds or burns Who is most at risk? People with compromised immune systems are at greater risk for sepsis, such as “The very young, the elderly and any people who may have conditions that suppress your immune system,” said Dr. Gonda. “For instance, if you have diabetes or if you’re an organ transplant patient who is on immunosuppressant therapy, you’re at somewhat higher risk.” Sepsis is often considered a hospital-acquired infection, but a study in The Journal of American Medical Association found that 80% of sepsis cases occur outside of a hospital. That’s why it’s especially important to remember any infection can lead to sepsis, and anyone can develop sepsis from an infection. What do I do? Timing is critical in the case of sepsis and septic shock. According to a study on septic shock patients, there is a 7.6 percent decrease in survival for each hour treatment is delayed. On the other end, if treatment is given within an hour of the first drop in blood pressure, the survival rate is 80 percent. Because sepsis can be so deadly, it’s important to seek medical attention as soon as possible. “If you’re not getting any better, if you think symptoms are progressively worsening – you should definitely be evaluated by a doctor,” said Dr. Gonda. You can help #StopSepsis by getting involved at worldsepsisday.org.
-
Cancer Support FAQs: How to Help When It's Someone You Love
Every cancer journey is different — and so are the ways individuals deal with a cancer diagnosis. So if you’re a close friend or family member, how can you help? Bobbi Gillis, manager of cancer support services with Renown Institute for Cancer, explains more. Just as we are all unique, we all also have our own ways of dealing with difficult news. For some, receiving a cancer diagnosis is devastating, and they want family members rallying around them in support; for others, they want to be left completely alone. So how do you know what is helpful and what is hurtful? For advice, we reached out to Bobbi Gillis, manager of cancer support services with Renown Institute for Cancer. Support, Defined What are some ways to support a loved one when they find out they have cancer? First and foremost, let them know you are there for them. As we can all imagine, a cancer diagnosis is scary, and it’s helpful just to know you have support if and when you need it. Second, try to listen and give advice only when you are asked. In trying to help as much as possible, many family and friends take on the role of “researcher” to find out more treatment options, but it’s best to avoid saying “you should try this” or “you ought to do that.” Patients are already dealing with a lot of information at once from care providers and their own research. You don’t want to make them feel overwhelmed or question the treatment they’re planning. What are some words of encouragement or support people can use? Just as you would in any difficult situation, speak from the heart and be genuine. But also be careful not to show false optimism or to tell them to just stay positive; saying these things may discount their fears and concerns. Here are some ideas to get you started: “We’re going to get through this together.” “Count me in to help out.” “I’m not sure what to say, but I want you to know I care and I’m here.” What resources are available to patients? What about their families? For patients with cancer, we offer support groups in-person or online. There are also support groups specific to the type of cancer you or your loved one have. You can check these out on our website, renown.org, or ask your care provider. There are also support groups and emotional support services available for family and friends. How can family and friends help throughout cancer treatment? It’s great to offer help, but it’s important to be specific when you offer. Saying “call me if you need something” is very general, and people may feel like they’re putting you out when they do ask for something specific. Instead, offer help with certain tasks — like driving them to treatment, babysitting, making them dinner or buying groceries. As much as possible, keep things normal. For some patients, being able to do everyday things like walking the dog helps them feel better. Loved ones can try to do too much for a patient, and while well-intentioned, this can make them feel less useful after being diagnosed. Renown Institute for Cancer | 775-982-4000 At the Renown Health Institute for Cancer, our experienced team provides the support and care to maintain the highest quality of life and then achieve the best possible outcome, all in one location that’s close to home. Our dedicated team, clinical expertise and advanced treatment options allow us to tailor care to each patient. Learn about: Our Team Cancers We Treat Screening and Prevention Treatment Options Find a Doctor
Read More About Cancer Support FAQs: How to Help When It's Someone You Love
-
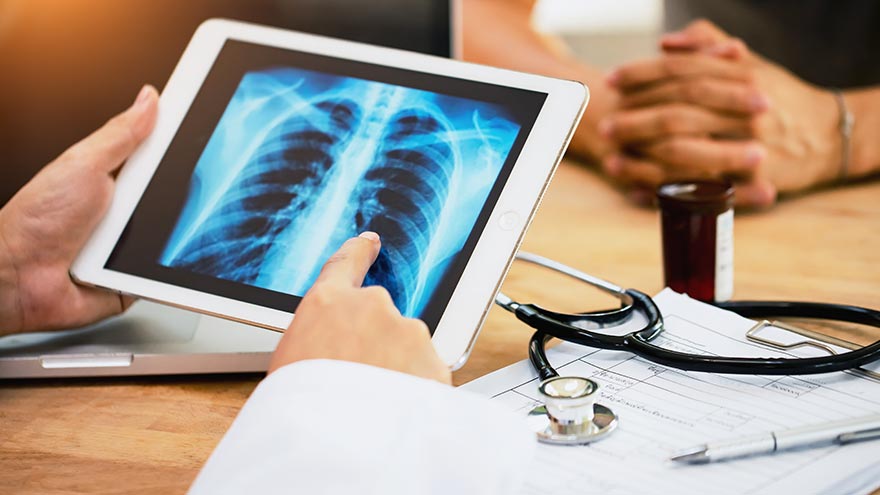
Lung Cancer Screening and Early Detection
Lung cancer is the leading cause of cancer deaths in both men and women in the U.S. The good news is the five-year survival rate increases dramatically if lung cancer is treated before spreading to other parts of the body. Julie Locken, MD, of Renown Health Imaging, explains more. What are the signs and symptoms of lung cancer? As you might expect, most lung cancer symptoms appear in the chest and can affect your breathing. Watch for signs such as: Persistent cough Constant chest pain Shortness of breath Wheezing Bloody or rust-colored phlegm Hoarseness Swelling of the neck Pain or weakness in the shoulder, arm or hand Recurring pneumonia, bronchitis or other lung infections Loss of appetite and loss of weight can also be signs of lung cancer That said, there are usually no symptoms in the early stages of lung cancer, which means getting screened can truly be a lifesaver. If you have a history of smoking, you should get screened as a precaution. What are the risk factors of lung cancer? Around 80% of lung cancer cases stem from a history of smoking tobacco. But there are other known causes, such as secondhand smoke, radon, asbestos and diesel exhaust. It’s important to do what you can to eliminate exposure to all of these to reduce your lung cancer risk. People with an immediate relative – a parent, sibling or child – diagnosed with lung cancer and people between 50 and 80 years old are also at higher risk and may need to consider screening. People who are at the highest risk are those with a history of smoking tobacco, particularly smokers who averaged one pack of cigarettes per day for 20 years or more, as well as former heavy smokers who quit in the last 15 years.
-
Dave's Story: How One Ranger Drove On
Meet Dave Pierson and his Wife Kathy Dave Pierson, 73, and his wife Kathy were just ten days away from a celebratory retirement trip to Africa in May 2021 when severe leg pain and discomfort landed Dave in the Veterans Administration (VA) Hospital. Unbeknownst to the couple, they would not be making the trek to Africa, and it would be several weeks before Dave would be back home with his wife in Carson City, their life drastically different than before. It all happened so fast. After a prompt referral from the VA Hospital to Renown Regional Medical Center, Dave received treatment for a bacteremia infection and underwent emergency spine surgery due to an epidural abscess. However, once his surgeon Edward Perry, MD completed the emergency procedure at Renown Health, Dave learned there was still a long road ahead. He had extremely limited body function and would need to learn to walk again. A Husband, Baseball Fan and Veteran Until this emergency spinal cord surgery, Dave had lived an especially healthy life in his retirement, traveling the world with Kathy, taking photographs along the way and attending ball games for their beloved team, the Reno Aces. Dave, a Vietnam veteran, and Kathy planted their roots in Carson City surrounded by countless friends and family, eagerly awaiting Kathy’s retirement. The Long Road Ahead It was those same friends and family who remained by Dave’s side throughout his recovery process. At the advice of the Renown team, Dave began a personalized physical rehabilitation plan at Renown Rehabilitation Hospital just days after his initial surgery. It was with the help of Charles Krasner, MD, an Infectious Disease Specialist that Dave made a smooth transition to be cared for at the Rehabilitation Hospital. Dave spent six weeks of inpatient treatment relearning fundamental occupational skills and motor functions such as eating and drinking, getting dressed, using a wheelchair and eventually taking his first steps, aided by a walker. The couple proudly remembers a day at the Rehabilitation Hospital when Dave successfully buttoned up his shirt using a small apparatus designed to aid in the task. "It was a little thing, but it was a monumental thing," Kathy shared. Dave achieved physical and cognitive victories, both on a small and large scale, over the next six weeks. Kathy visited every day she could, always prepared with a photo of the couple's past travels to encourage Dave. The Rehabilitation Hospital staff grew close with the Piersons, sharing stories and photos of their dogs, travels and life. The nurses kept Kathy updated about her husband’s condition and prepared her for the journey to come, this included extensive education related to Dave’s future at-home care. Benjamin Pence, MD, Dave’s lead rehabilitation doctor and the Director of the Institute for Neurosciences, always seemed to know just how to motivate Dave on his most challenging days. As a ranger in Vietnam, the phrase, “drive on ranger” meant a lot to the veteran when it came to determination and perseverance. So, the phrase was used as encouragement by Dr. Pence and the Rehabilitation Hospital team throughout Dave’s journey, becoming a fond memory about hope and determination during recovery.
-
Heart Care
We lead the region in cardiology care with our technological expertise and patient-centered approach. Our comprehensive team diagnoses heart disease and other cardiac conditions, offering personalized treatment plans. Plus, our specialty team provides you access to the most advanced medical, surgical and minimally invasive techniques.
-
Clubfoot An Unexpected Story of Expert Baby Care
A clubfoot is where the foot is turned in on itself and points toward the ground. A clubfoot diagnosis during pregnancy is surprising and challenging during any circumstance. And in the case of parents anticipating surgery during a pandemic, options can be scarce. These parents took a deep breath, and with the help of Michael J. Elliott, MD, pediatric surgeon with Renown Children’s Hospital, their baby is on the road to recovery.
Read More About Clubfoot An Unexpected Story of Expert Baby Care
-
Name-Brand Medication vs. Generic: What's the Difference?
Most prescriptions meds are available in generic form. Find out the similarities and differences between the two and how to determine whether a generic is right for you. Approximately 80 percent of prescriptions sold today are generics. If you’re taking a prescription medication, chances are it’s a generic form of the brand-name drug. But are you getting the same quality in a generic medication? Do generics measure up? The answer in most cases is yes — generics, just like branded products, are regulated by the Food and Drug Administration. “To have a generic product approved by the FDA, the generic manufacturer must prove that its product is bioequivalent to the branded product,” explains Adam Porath, PharmD, BCPS AQ-Cardiology, BCACP and Vice President of Pharmacy Services. Basically, it has to function the same. “Generic products are extremely well tolerated and will provide the same results as using a branded product,” Porath says. Here’s how generics are the same as name-brand prescriptions: Generic products contain the same active ingredients. They produce the same desired clinical effect and accompanying side effects. Generics come in the same form as their branded counterparts: pill, liquid or inhaler, for example. Release into the bloodstream matches the name brand in timing and strength. Here’s how they differ: Generics generally cost less. Federal law requires generics have different names and look different: shape, size, markings and color. Generics contain different inactive ingredients, like binders, fillers and artificial colors. Different side effects with generics can usually be attributed to these additions. Why do generics cost less? When pharmaceutical companies develop a new drug, they are paying for research, development, clinical studies, marketing — in some cases it can cost more than $800 million and take 10 to 15 years to develop a new drug. “The manufacturers of branded medication products have to recoup their research and development costs,” Porath says. So companies are granted a limited patent to sell their drug without the competition of generic counterparts. “When patent exclusivity ends, the market is open for any generic manufacturer to make a competing product with FDA approval.” Without the same startup costs, companies can sell generics at 80 to 85 percent less. And because more than one company can produce the same generics, competition drives prices even lower.
Read More About Name-Brand Medication vs. Generic: What's the Difference?
-
OBGYN in Reno/Lake Tahoe
Full Time - Eligible for Benefits510701 AdministrationVaries -
Physician_Rheumatology
Full Time - Eligible for Benefits510701 AdministrationDay