Search
Results for 'jobs'
Clear-
One Patients Story of Survival
Thanks in part to the care provided by Renown’s award-winning team of ICU nurses, Tony Mowatt is alive, thriving and engaged. Read his story — and learn about the exclusive Beacon Award of Excellence — below. The open road. The growl of the engine. The feeling of freedom. That’s what Oakland resident Tony Mowatt was enjoying as he drove up Highway 88 toward Reno for the semi-annual Street Vibrations event. But he wasn’t expecting to hit the diesel truck — or to fly off of his bike over 100 yards, skidding onto the side of the road. He was severely injured and in the midst of rural Nevada. He had crashed just outside Centerville, Nev., and was miles away from any critical care hospital. Having the only trauma center equipped to treat his serious injuries, Tony was flown to Renown Regional Medical Center and admitted to the intensive care unit (ICU). ICU Nurses Treat Patient, Support Family Tony’s girlfriend, Tasha Klubock, was notified by his friend that he had been taken to the hospital. She immediately drove from Oakland to Reno to see Tony at Renown. Her first night there was overwhelming and scary — nobody knew if Tony was going to survive. But the nurses helped Tasha cope with the initial shock. Caring for the patient isn’t their only job — they also care for the family. “They [the nurses] just kept coming in and checking on me,” she said. “Angela was so amazing that first night. I really just bonded to her, and I remember when the shift switched, I panicked thinking about who was coming on and wanting to meet the next nurse … But they all came to talk to me — I had updates from everybody. It was just amazing.” ICU Nurses Became Family Tony spent 32 days in Renown’s Sierra ICU, surviving a serious head injury, all with Tasha by his side. He and Tasha still stay in touch with Renown nurses. “Even though this was literally one of the most hideous, craziest things to go through,” Tasha said. “There was so much hope and they became such a family to me and I still think of that time fondly because of the nurses.” “I’m alive because they wanted me to be,” Tony said. And Tony and Tasha are now happily engaged and planning their wedding. Exceptional Care: Renown ICU Nurses Win Awards Renown’s ICU nurses provide care like this every day to countless patients — it’s so second nature to them that they forget how exceptional it truly is. But it’s certainly care like Tony’s that has earned them national recognition. The American Association of Critical Care Nurses awarded the Beacon Award of Excellence to the Sierra, Cardiac and Roseview ICUs. These are the only ICUs in Nevada to obtain this honor. The Beacon Award recognizes critical care nursing teams who exemplify excellence in areas like leadership, process systems, quality care, knowledge, learning and development, excellence in patient care and superior patient health outcomes. “I couldn’t have been more proud of what we’ve done to accomplish this,” said Nick Dovedot, Cardiac ICU nurse. “It represents who we are. Just a great group of individuals who all work together as a team to make our patients get better.”
-
Bladder Control Treatment for Women – What’s Right for You?
Although going to the bathroom is not a typical conversation among women and their doctors, it’s an important one. It is a topic you may want to discuss with a urogynecologist, a physician who diagnoses, manages and treats pelvic health conditions in women. Kerac Falk, MD, a urogynecologist and assistant professor at the University of Nevada, Reno and Renown Health discusses overactive bladder in women and how to treat it. According to the National Institutes of Health, about 1 in 4 women struggle with pelvic health conditions, with over 40 percent of women over age 60 experiencing problems. While these conditions may be common, they shouldn’t just be accepted as a normal part of getting older. In fact, many women don’t think of urine leakage as a medical problem, and only 1 in 3 women with incontinence seek care. So, while these conditions may be common, they shouldn’t just be accepted as a normal part of getting older. There are excellent treatment options that can significantly improve the quality of life. Overactive Bladder Symptoms in Women: As your body changes and ages, so does your pelvic health. Whether you just had a baby, are experiencing urgency issues or find you cannot go about your daily routine, sneeze or laugh without leaking urine – you’re not alone. An overactive bladder, also known as OAB, is more than feeling an urgent need to go to the bathroom. It can also include the following: Incontinence or lack of control over urination Waking up in the middle of the night to empty your bladder Going to the bathroom often, even every 30 to 60 minutes Symptoms of OAB can lead to a decreased quality of life, feeling as if you cannot go about your normal daily routine, or even become hazardous, increasing the risk of trips, falls, and bone fractures. Various Treatments are Available: Behavioral management (eliminating coffee, soda and alcohol which irritate your bladder) Pelvic floor physical therapy to optimize nerve and muscular function and coordination to prevent leakage Medications including tablets and local estrogen replacement Pelvic nerve stimulation and reprogramming treatments Botox to relax the bladder muscle Solutions for an Overactive Bladder: Simply put, OAB is a nerve and muscle problem, so the bladder needs to calm down. Although there is no underlying reason for OAB, some underlying conditions may exist, such as: High blood pressure Recent trauma Neurological conditions (such as stroke and multiple sclerosis) Lifestyle and non-invasive measures can usually reduce symptoms by as much as 50%, significantly improving quality of life. However, if these measures do not help your OAB, further bladder testing may be needed. Dr. Falk notes that “every patient has a unique situation and set of symptoms. My job as a urogynecologist and pelvic floor subspecialist is to work as a team with each individual to figure out what’s going on and design the best treatment approach that fits your needs and goals, whether that is conservative or with more advanced procedures. The outcome we are working towards is improved quality of life.” If you are bothered by your bladder, the best thing you can do is bring this up with your primary care doctor or gynecologist to begin to discuss solutions
Read More About Bladder Control Treatment for Women – What’s Right for You?
-
Suicide Risk How to Spot a Friend in Crisis
How can you tell if a friend is in trouble or struggling with suicidal thoughts? And how can you support them in finding help? Are you feeling virtually exhausted? Life is always challenging, but the mental fallout of a global pandemic is real. Contributing to the loneliness epidemic is the shifting American lifestyle. More Americans live alone (28%) now than ever before, and fewer have kids. First, let’s acknowledge this is a time of anxiety and worry for everyone. Economic uncertainty, job transitions, grief, and loneliness are a perfect storm for mental stress. Even before the COVID-19 (coronavirus) pandemic mental health was a concerning issue, now it is a relevant topic of crisis. Secondly, anyone can struggle with suicidal thoughts. Those suffering from drug addiction are especially vulnerable. In particular the U.S. is currently seeing a rise in drug overdoses by almost 18% due to the pandemic. Unfortunately, suicide is responsible for one U.S. death every 11 minutes, according to the Centers for Disease Control and Prevention. Not to mention the millions who think about it, make a plan or attempt it. It is important to remember that suicidal thoughts, plans or intent must be helped immediately. Understanding Suicide Risk To clarify, depression is not a choice. No one wishes for endless days of feeling down, sleepless nights, and feeling as if you are in a dark tunnel. Currently, one in five Americans will experience a mental illness this year. This means one of your friends is struggling, right now. Specifically, consider this: When your body feels pain it talks to your mind. When your mind is suffering who does it talk to? So, how can you tell if a friend is in trouble? According to the National Institute of Mental Health be on the lookout for some depression clues below. Signs and Symptoms of Depression Persistent sad, anxious, or “empty” mood Feelings of hopelessness, or pessimism Irritability Loss of interest or pleasure in hobbies and activities Decreased energy or fatigue Moving or talking more slowly Feeling restless or having trouble sitting still Difficulty concentrating, remembering, or making decisions Signs and Symptoms of Suicide Risk Expressing feelings of hopelessness or having no purpose Talking about feeling trapped or being in unbearable pain Talking about being a burden to others Increasing the use of alcohol or drugs Sleeping too little or too much Withdrawing or isolation Displaying extreme mood swings. Talking about wanting to die or to kill oneself (Reference: Suicide Awareness Voices of Education) How to Help a Suicidal Friend It can feel awkward to approach the subject of suicide with a friend, but take any of the above warning signs seriously. Other ways you can help are by: Encouraging self-care and making sure they take care of basic needs Listen to their worries without judgement Ask them what they need from you, then follow through with action Let them know they are not a burden Don’t minimize or invalidate their feelings Point them to helpful resources Be their advocate and get them help If someone you know is in a life-threatening crisis situation, call 911 immediately. Suicide Risk Resources: National Suicide Prevention 24/7 Lifeline: 1-800-273-8255 Ayuda En Español: (Spanish National Suicide Prevention Lifeline) 1-800-628-9454 Crisis Text Line: Text HOME (or CONNECT) to 741741 to chat with a crisis counselor 24/7 free of charge. The National Alliance on Mental Health: 1-800-950-6264 Substance Abuse and Mental Health Services Administration: (SAMHSA) 24/7 helpline 1-800-662-4357
-
From Renown NICU Nurse to NICU Mom: Mariah DaSilva’s Inspiring Journey
Located on the 5th floor of the Tahoe Tower, Renown’s newly updated Level III Neonatal Intensive Care Unit (NICU) is decorated with colorful artwork on the walls, the lights dim for the newborns resting, and parents conversing next to the bassinet with nurses on their baby’s journey to health. In the quiet, shuffling hallways stands Mariah DaSilva, a Renown NICU Nurse, whose own birth story showed her true compassion and professional dedication to what it means to care for the tiniest and most vulnerable patients. From the Medical Floor to the NICU Mariah started her nursing career on the medical floor at Renown; however, after a year, she was excited to see her dream job open in the NICU and helping to provide compassionate care for the most fragile patients. “I’ve always known that I wanted to work with babies so being a NICU nurse was a dream of mine,” said Mariah. “I truly love what I do, and I can’t imagine being anywhere else than the NICU.” A high-stakes environment, the NICU is where babies are transferred to after birth when they require medical intervention. They care for babies as young as 23 weeks gestation, up to full-term babies. Any babies born less than 35 weeks are automatically admitted into the NICU for treatment. Other than prematurity, babies can be admitted to the NICU for respiratory distress, low blood sugar (hypoglycemia), cardiac anomalies, birth defects, seizures and other medical conditions that need treatment or assessment. A Day in the NICU: The Heart of Care A typical day for Mariah starts with reviewing her assignments and receiving a detailed report from the night shift. Preparing for the day involves scrubbing in and wiping down patient care areas to maintain a clean environment. Once everything is set, she begins a series of scheduled care tasks, which include performing assessments, feeding, changing diapers and facilitating parent involvement in their baby’s care “There are so many exciting ‘firsts’ that happen in the NICU; parents holding their baby for the first time, parents' first time changing their baby’s diaper, bathing their baby for the first time, first time breast-feeding or bottle-feeding, the baby’s first time taking a full bottle, watching a baby breathe on their own without any respiratory support, etc.,” said Mariah. “There are so many big milestones that happen in the NICU that I am so incredibly lucky to be a part of.” The NICU nurses work closely with neonatologists, nurse practitioners, respiratory therapists, speech therapists, physical therapists, occupational therapists and other specialists to deliver comprehensive care. This teamwork and collaboration ensure that each baby receives the best care possible for their health journey. Mariah shared a reflection on her team: “Our NICU team is amazing. Being a part of a team that is so compassionate and collaborative is amazing. We all work closely together to ensure we’re providing the best care possible for every single baby that comes to the NICU. We are all very protective of the babies that we care for in the NICU and truly want the best outcomes for them and their families. Taking care of such a vulnerable population comes with a lot of responsibility and we take pride in what we do each day.” As with all healthcare professionals, NICU nurses require immense strength and compassion to care for the youngest patients in a highly sensitive environment. “More often than not, we have really good days in the NICU, but we also have really hard days that affect every single person in the NICU,” said Mariah. “The loss of a baby, delivering bad news to a parent, an extended NICU stay and a baby withdrawing from drugs are all situations that we unfortunately deal with in the NICU. These situations are all very challenging, but we have to stay strong for the babies and their families.”
Read More About From Renown NICU Nurse to NICU Mom: Mariah DaSilva’s Inspiring Journey
-
Mammography Technologist
Per Diem - Non Benefited209259 Imaging 910 VistaDay -
Mammography Technologist
Per Diem - Non Benefited400749 OP ImagingVaries -
Mammography Technologist
Sign On Bonus - up to $30,000Full Time - Eligible for Benefits209259 Imaging 910 VistaDay -
Mammography Technologist
Per Diem - Non Benefited209257 Imaging Breast HealthDay -
Department Spotlight: Respiratory Care
This Department Spotlight is dedicated to Jason Simpson, Manager of Respiratory Services at Renown Children’s Hospital. Take a moment to breathe deeply. Inhale in, exhale out. We rely on our lungs to provide us with the air we need to live a healthy life – and this essential bodily function is something that many of us don’t think twice about since it comes easily for us. Now, imagine yourself as someone who is living with severe asthma, chronic obstructive pulmonary disease (COPD) or someone who was recently diagnosed with a frightening respiratory condition like COVID-19 or pneumonia. The simple act of breathing can prove to be an intimidating venture requiring the care of a professional. Who are the people that take on the challenge? Meet Renown Health’s Respiratory Care Services department. Serving patients across 13 service lines, three acute facilities, outpatient locations and telehealth, our respiratory specialists – including respiratory therapists, respiratory care aides, inpatient COPD respiratory therapy navigators and educators and more – use their expertise to help restore the vitality of all their patients with every inhale and exhale, shaping a healthier livelihood one lung at a time. The Guardians of Respiratory Wellness Whether they are managing lifelong respiratory conditions or offering crucial support in emergencies, the Respiratory Care team strives to enhance the quality of life for every patient. As an indispensable member of the clinical team at Renown, our respiratory therapists work collaboratively with doctors and nurses to tackle a wide range of tasks, tailoring care for each patient’s unique needs. “Respiratory care is involved with all stages of life, from beginning to end,” said Sarah Kurtz, Respiratory Therapist. “We work closely with nurses and doctors and perform arterial punctures, breathing treatments, weaning maneuvers for patients on life support, intubations and much more. We assess patients constantly to see if their care needs to be upgraded or if they can be weaned to get them back home with their families.” “You start your morning researching your assigned patients,” added Tim Start, Respiratory Specialist. “We go over lab values and chest radiographs and decide the best plan of care for each patient. Our objective is to improve their respiratory status by giving them medications and doing breathing exercises. We participate in other forms of care with nurses, such as activities of daily living (ADLs) and mobilization. We work as a team, and that enables us to provide great patient care.” For patients living with COPD, enjoying all that life has to offer comes with a separate set of obstacles. According to the Centers for Disease Control and Prevention (CDC), over 200,000 people across the Silver State are living with this chronic condition. Luckily for them, Renown has a specialized team to help these patients optimize their life and manage their condition with individualized treatment and education. “We run a report every morning to identify all the patients currently admitted who have a history of COPD, take respiratory medications or smoke,” said Amber Beck, Inpatient COPD RT Navigator. “After looking through their charts, we visit with the patient (and possibly their family) at the bedside to help them better understand how to manage their breathing issues.” As a vital part of the Respiratory Care team, Renown’s respiratory care aides help ensure the seamless operation of our respiratory care services. These dedicated professionals provide essential support to respiratory therapists not only during intricate procedures but also outside of face-to-face patient care by transporting equipment, restocking supplies, assisting in the mobilization of patients and more. “We are responsible for the maintenance of unit supplies and making decisions regarding levels of stock to be maintained,” said Dia Ramos, Respiratory Care Aide. “We also transport equipment, refill the oxygen tanks on the floors and intensive care units (ICUs), order and stock respiratory care supplies, mobilize patients and assist the respiratory therapists during bronchoscopies in the ICUs. In addition, we clean respiratory equipment like mechanical ventilators, continuous positive airway pressure (CPAP) and bilateral positive airway pressure (BiPAP) machines, high flows and aerosol poles.” Once the COVID-19 pandemic hit, a special spotlight shined upon respiratory care teams across the country for the heroic care they provided patients in respiratory distress. While their roles in health systems have gained a better understanding nationwide, this team understands it is vital for them to educate the community about the important jobs they hold for our patients. “Respiratory care can be under the radar,” said Pam Umek, Respiratory Specialist. “Once, when I told someone that I am a Respiratory Therapist, they said, ‘Oh, like a yoga breathing instructor?’ I then explained all the things we do: intubation, extubation, bronchoscopies, transports, traumas, codes, rapid responses, pediatrics/NICU, breathing medications/therapies, open heart rapid ventilator weaning … needless to say, that individual walked away with a better understanding of not just Respiratory Care Services but also the enormous effort it takes to care for our community.” The accolades and achievements continue to pour in, from national awards and certifications to implementing different jobs in care units to optimize the patient care experience. “We have earned and continue to maintain the Joint Commission Disease-Specific Certification for COPD,” said Amber Beck. “We are well below national averages for 30-day readmissions, lengths of stay and mortality due to COPD. Sandy, one of our COPD Coordinators, was a recipient of a patient advocacy award from the American Association of Respiratory Care and FACES Foundation.” “We have started implementing Respiratory Care Aides in the critical units, starting with the Cardiac ICU,” added Dia Ramos. “We work as one team and are always helping each other with their tasks.” Education and mentorship are at the core of Renown’s mission to make a genuine difference in the health and well-being of every patient. Nurturing the next generation of medical professionals – including respiratory care professionals – is a task that the Respiratory Care team takes seriously. “It has been great being able to help educate students in different disciplines,” added Pam Umek. “We have been able to offer shadow shifts to students in emergency medical services (EMS), nursing and medical school. These opportunities help students entering the medical field have a better understanding of the many ways we can help care for our respiratory patients.” From the moment of birth to the final stages of life, Renown is fortunate to have a Respiratory Care team that tirelessly ensures every breath counts, safeguarding their role as a trusted partner within our health system. A Tribute to Jason Simpson, Healthcare Hero
-
Information Security Specialist - Badge Information Specialist
Full Time - Eligible for Benefits100550 Renown Health-SecurityDay -
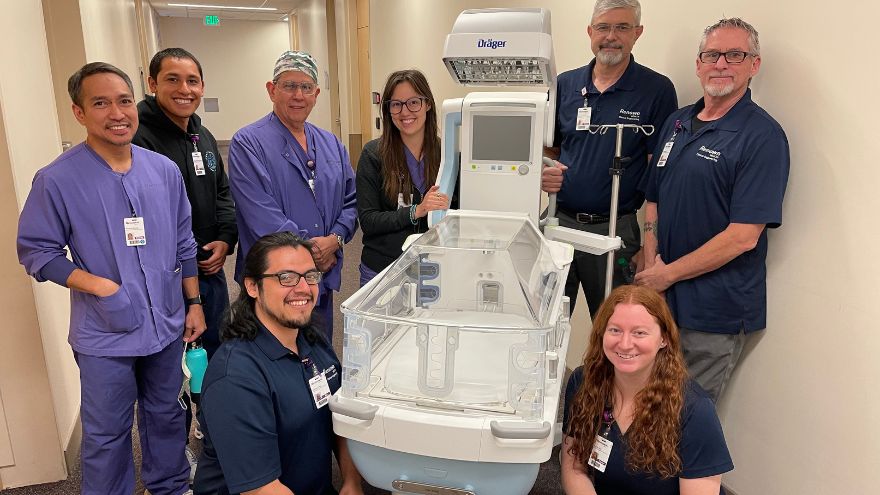
Department Spotlight: Clinical Engineering
Renown Health strongly supports and advocates for innovative medical technology. Our diverse lineup of medical equipment enables our care leaders to provide quality care to every patient. But what if a piece of technology breaks down? What happens when our care teams are ready for technological upgrades? Where do employees go when they have a question about a complicated piece of equipment? Enter the Clinical Engineering department. This sophisticated team is staffed with intelligent, science-minded individuals who are ready to jump in and help at any given second. From newborn incubators to robots that clean the hospital floors, these team members are the med-tech masters that keep our health system running. Equipment Experts Upon entering the Clinical Engineering department’s workshop, you are welcomed with an abundance of high-tech equipment undergoing repairs and upgrades. The department takes care of more than 26,000 pieces of equipment throughout the entire healthcare network, including the technologies at the University of Nevada, Reno School of Medicine, which they just took over this past year. To the average person, this may seem overwhelming; however, for this team, this is the exact environment they thrive in to make the technology magic happen. “I am motivated and engaged every day at work,” said Tony Martinez, Supervisor of Clinical Engineering for Renown. “Our department is fast-paced and rewarding, and that’s a big plus.” While some team members enter the department as equipment generalists, this team offers training to develop their skills on certain pieces of equipment, eventually becoming specialists. “Every month, we encourage our colleagues to undergo specific training on more delicate equipment,” said Tony. “Once we get to that point in their training, we assign different equipment to our team members every month. They pick up the experience very quickly.” As a Clinical Engineering Technician for Renown, Rylie Nickerson took advantage of the training and educational opportunities offered to her and is now a ventilator specialist especially for Renown’s neonatal intensive care unit (NICU). “Regardless of whether I’m working on ventilators or on another piece of equipment I’m assigned to, I’m always thinking about how I can help the patients, nurses and doctors,” said Rylie. Raul Hernandez, a Clinical Engineering Specialist for Renown, is the go-to person for anesthesia, heart-lung bypass, red cell saver and life support equipment. He embraces the fact that, regardless of whether you are a specialist or a generalist, there is no typical day working in this department. “Every day brings different challenges,” said Raul. “I really enjoy the mental exercises I do every day. They keep me grounded and focused.” On top of their day-to-day work and any special projects or emergencies that come up, the team is on an ongoing preventative maintenance schedule. Think of this work like your car’s oil change – routine maintenance to prevent something from breaking down in the future. “At any point, we might have 100-200 extra pieces of equipment to handle during preventative maintenance,” said Taylor Gray, a Clinical Engineering Technician for Renown. “We are always helping each other through any issues.” Our Clinical Engineering team shows exactly what it means to be collaborative. Even though their to-do lists are ever-growing, this team never feels alone. They know they can always lean on each other for support, regardless of the workload. “We always have each other’s backs,” said Taylor. “I feel so happy and satisfied in my job, and my coworkers are a large part of that.” Celebrating the Genuine Difference The Clinical Engineering department is driven by their desire to help and take care of the entire health system, and in turn, make a genuine difference for the communities we serve, from the medical staff to the patients. “The satisfaction you get in our field when we impact patients’ lives and their healing process is so motivating and engaging,” said Tony Martinez. “It’s a great feeling.” The team knows the common saying ‘Walk a mile in someone’s shoes’ very well; so well, in fact, that they take it to the next level, doing everything they can to prevent frustrations and extended down times. “We try to walk a mile in someone’s shoes before they get angry,” said Reagan Jordan, Director of Clinical Engineering for Renown. “Your satisfaction is our mission, and our team continually works to improve their outcomes every day.” This department is where the entrepreneurial spirit and science-focused mind meet. For people like Raul Hernandez, who came from a business background as well as decades of medical technology experience, Renown helps him bring both his personal and business skills into focus. “This environment is very beneficial for Renown, me, and of course, the patients,” added Raul. Being members of a team that is committed to excellence and purpose inspires them to reach new heights in patient care. “I am constantly reminded of the positive impact we have by witnessing the individual experiences we have and hearing the enthusiasm and thankfulness in their voices,” said Raul. “It gives me a great sense of pride to work at Renown.” "There is a strong feeling of mutual respect here,” added Ed Trejo, a Clinical Engineering Technician at Renown. “We are always here to help.” The proof is in the data. The Clinical Engineering team scored as one of the top departments in the recent Renown employee engagement survey, with their results sitting at more than 94 percent. “This speaks to not only our department leadership but also the team as a whole,” said Reagan. “I am extremely proud of them. Despite the pandemic, they are knocking it out of the park.” For this department, coming to Renown is easy; staying at Renown is even easier. “Staying at Renown is the easy choice,” said Raul. “And this team is only going to grow.” Workflow Whizzes and Kindness Champions “Rolling with the punches,” as Tony Martinez says, comes naturally to the Clinical Engineering team. With the constant workflow of equipment coming into the shop, every team member has learned how to be experts at prioritizing, especially based on the needs of our organization. Even though their jobs can bring a lot of intensity, this department’s positive attitude radiates throughout the hospital. Upon entering the workshop, everyone is greeted with a smile from every team member, along with an immediate willingness to dive into the complex world of engineering. “The experience of helping other people with their unique needs is invaluable,” said Taylor Gray. If this work environment sounds enticing, great news – the Clinical Engineering team is growing. Motivated, aspiring engineers with a passion for healthcare and an associate’s degree in a related field are welcome. Military experience is also valued very highly in this team. As many of our military servicemen and servicewomen gain specialized engineering experience while enlisted, the military-to-engineer career ladder at Renown is especially strong. In fact, according to Paul Joseph, a Clinical Engineering Technician at Renown, the majority of their teammates come from a military background. Above all, being capable of prioritizing on the fly, thinking critically, having an open-mined outlook and being self-driven are the top skills that this department values. As Ed Trejo states, “If you’re willing to wear different hats, you will do very well here." “Go with the flow, and expect the unexpected,” added Rylie Nickerson. Those who join this team feel at home. The warm embrace of the team’s kind nature and the supportive environment they all foster inspires an efficient workflow that helps our entire hospital system function at the top of its game. At the end of the day, everyone who joins the team, or anyone who even interacts with the team in any capacity, will be in good hands. Mandy Noriega, a Clinical Engineering Technician for Renown, closes these thoughts with a great reminder to each and every one of us: “After all, teamwork makes the dream work.”