Search
Results for 'doctor'
Clear-
Renown Launches Virtual Symptom Checker
Renown Health just announced a new, digital tool designed to keep our community safe and healthy. Symptom Checker, which launched today, is a user-friendly, web-based platform that assesses patients’ symptoms and seamlessly directs them to the appropriate level of care within the Renown network. Symptom Checker can be accessed 24/7 by visiting Renown Symptom Checker. From there, a patient can identify the area of the body responsible for their discomfort, and specify their symptoms. Upon entering their symptoms, patients receive a detailed health summary and care guide, which helps them determine the most appropriate action to take. Patients are able to schedule a visit at a Renown location directly through the Symptom Checker portal. Patients experiencing a medical emergency should not use Symptom Checker and instead call 911. “Thanks to Symptom Checker, our patients will have around-the-clock support at their fingertips to help them make informed decisions about their healthcare needs,” said Tony Slonim, MD, DrPH, President and CEO of Renown Health. “We understand that determining the right level of care for you or your loved ones may bring about some uncertainty, which is why we are proud to continuously offer new and innovative technologies that make it easier for our community members to live healthier lives.” “As we continue experiencing cases of COVID-19 in Washoe County, many individuals with COVID are unsure when they should seek medical care, as well as the appropriate location to receive care,” said Melodie Osborn, RN, Chief Quality and Nursing Officer, Health Services. “With Symptom Checker, people can easily input their symptoms, and include the symptom severity, to be directed to the best level of care for their individual health needs—making it an extremely valuable tool as we fight to keep our community safe and healthy amidst this pandemic.” Symptom Checker is free to use and does not require users to be Renown patients. In addition to nearly 200 children and adult symptom care guides, the platform also features 55 first-aid topics, 147 parenting advice topics, and 25 over-the-counter drug dosage tables for children and adults. The Symptom Checker content is written by medical doctors, Barton Schmitt and David Thompson, who are nursing triage experts; and symptom care guides stem from clinical protocols used by doctors and nurses worldwide. Evidence behind the Symptom Checker can be accessed here. For more information, or to use Symptom Checker, please visit Renown Symptom Checker. About Renown Health Renown Health is a locally governed and locally owned, not-for-profit integrated healthcare network serving northern Nevada, Lake Tahoe and northeast California. Renown is one of the region’s largest private employers with a workforce of more than 7,000. It comprises three acute care hospitals, a rehabilitation hospital, the area’s most comprehensive medical group and urgent care network, and the region’s largest and only locally owned not-for-profit insurance company, Hometown Health. Renown has a long tradition and commitment to continually improve the care and the health of our community. For more information, visit renown.org.
-
Renown Children's Hospital
Renown Children's Hospital is proud to be northern Nevada's only pediatric hospital. The Renown Children’s ER is the region's only Level II Pediatric Trauma Center and is open 24 hours a day, seven days a week. With pediatric specialists, child-sized equipment and family-centered care, it’s the first and only facility of its kind in Reno-Tahoe. Whether your child requires a pediatric appointment, a sports physical, or emergency medical attention, our pediatric care is focused on providing compassionate support to both patients and families.
-
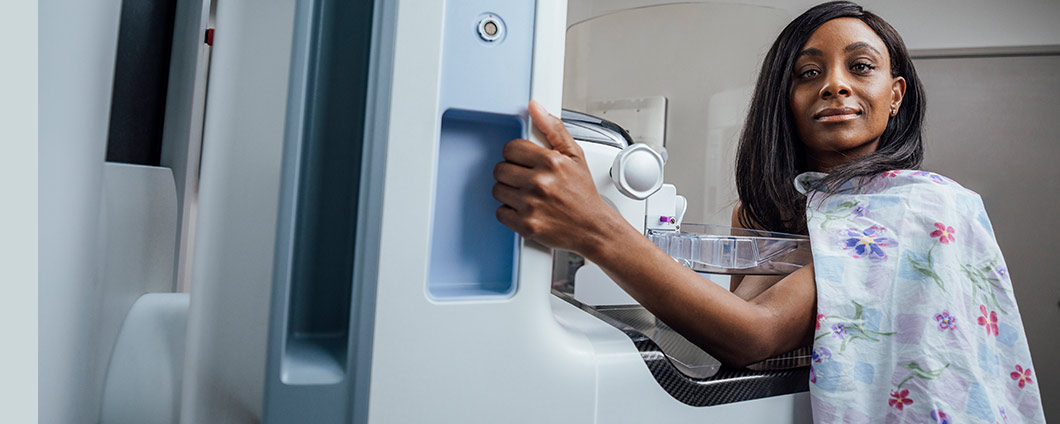
Mammograms
Breast Screening at Renown Women's Health: Because breast health is YOUR health. 1 in 8 women in the U.S. face a breast cancer diagnosis each year. Early detection through annual mammograms significantly increases the chances of successful treatment. At Renown Women’s Health, we provide expert, compassionate care, guiding you through each step of your mammogram. Our advanced 3D technology detects 41% more cancers and reduces false positives, lowering the need for rescreening. Join the thousands of women in northern Nevada getting screened and putting their health first. We offer mammograms at our four imaging locations in Reno and Sparks, Nevada, providing up to 40 daily appointments with short wait times.
-
How to Fight Cancer that Runs in the Family
Your mother had breast cancer. Your uncle had colon cancer. A cousin has stomach cancer. Could yours be the next name to make the family cancer list? “Possibly,” says Dr. Robert Nathan Slotnick, MD, PhD, Medical Geneticist at Renown Medical Group. In this article, the doctor discusses the genetics behind Lynch syndrome — and how you and your family can fight it. What is Lynch Syndrome? Lynch syndrome, also known as hereditary non-polyposis colorectal cancer (HNPCC), is one of the most common genetic conditions known to increase cancer risk in individuals and families. It enables colon and other cancers to develop by causing mutations in mismatch repair (MMR) genes. “The genes MLH1, MSH2, MSH6, PMS2 and EPCAM normally help to repair damaged DNA,” explains Dr. Slotnick. “But when they don’t work properly, naturally occurring DNA replication errors are not repaired efficiently. These errors accumulate and cancer can be the result.” Colon cancer is just one of many possibilities. People with Lynch syndrome also have a higher risk of developing endometrial cancer (cancer of the inside lining of the uterus) as well as cancer of the ovaries, stomach, pancreas, kidney, brain, and bile duct, among others. These syndrome-enabled cancers often appear in patients before the age of 50. Family Cancer Clues The family connection to cancer is a strong one notes the doctor. “Cancer is best considered a genetic disease because it is always tied to changes (or mutations) in our inherited material: our DNA,” says Dr. Slotnick. “These DNA changes cause cells to lose control of their normal constraints on growth and metabolism and can allow abnormalities to develop.” “Although all cancers are genetic,” he adds, “not all cancers are hereditary or passed down through generations.” But because Lynch syndrome IS a hereditary condition, personal and family cancer histories provide invaluable information toward diagnostic confirmation and to a path of surveillance, prevention and treatment. Once a strong family history of cancer is confirmed, doctors and geneticists can move forward with targeted genetic testing to identify specific gene mutations. If Lynch syndrome is diagnosed, testing can also reveal your risk for associated cancers. And your results could be a wake-up call to family members. According to the Centers for Disease Control and Prevention (CDC), close relatives of people with Lynch syndrome have a 50% chance of having similar gene mutations and a higher risk of cancer. The good news is detection and prevention progress is being made. “Lynch is just one of many cancer syndromes where risk is tied to heredity,” explains Dr. Slotnick. “In the last few years, our ability to identify those at risk for this type of cancer predisposition has improved markedly, both in diagnostic accuracy and cost. This allows us to provide aggressive surveillance and prevention choices to individuals and families at risk. Healthier families and lower cost: it’s a win-win.”
-
UnitedHealthcare & Renown Health Announce New Contract Agreement
New contract provides members with continued in-network access to all Renown hospitals and physicians UnitedHealthCare and Renown Health today announced they have reached an agreement on a new contract. The agreement protects affordability and value-based care, and provides UnitedHealthCare members with continued in-network access to all Renown hospitals and physicians. Renown Health President and CEO, Anthony Slonim, M.D., DrPH, FACHE, stated, “We appreciate the collaborative approach of both teams to reach resolution. As Nevada’s most preferred health system and Reno’s only not-for-profit health care organization, our mission is to make a genuine difference in the health and well-being of the community. As doctors, nurses and caregivers, we want to ensure the greatest access, experience and highest quality care for every member of our community, including those insured by UnitedHealthCare. Today’s agreement marks another important milestone in achieving the goals of our strategic plan and a healthier Nevada.” United contracts for all Renown Health services had terminated on June 1. The Health Plan of Nevada (HPN) contract remains to be negotiated and finalized. Consumers with questions can contact United by using the toll-free number on the back of their current United identification card. ### About Renown Health Renown Health is a locally governed, not-for-profit integrated healthcare network serving northern Nevada, Lake Tahoe and northeast California. Renown is one of the region’s largest private employers with a workforce of more than 7,000. It comprises three acute care hospitals, the region’s only children’s hospital, a rehabilitation hospital, the area’s most comprehensive medical group and urgent care network, and the region’s largest and only locally owned not-for-profit insurance company, Hometown Health. Renown has a long tradition and commitment to continually improve the care and the health of our community. For more information, visit renown.org.
Read More About UnitedHealthcare & Renown Health Announce New Contract Agreement
-
Health Insurance Terms Explained: HMO, EPO and PPO Plans
When it comes to purchasing a health insurance plan, you’ve probably heard of the two plan types, HMO and PPO, but what exactly do these terms mean, and what is an EPO? Let’s learn more about these plan types and how you can choose the plan that meets your needs. What is an HMO Plan? HMO stands for “Health Maintenance Organization.” HMO plans contract with doctors and hospitals creating a network to provide health services for members in a specific area at lower rates, while also meeting quality standards. HMO plans typically require you to select a primary care physician (PCP) and obtain a referral from your PCP to see a specialist or to have certain tests done. If you choose to see a provider outside of the HMO’s network, the plan will not cover those services and you will be responsible for all charges. What is an EPO Plan? An EPO stands for “Exclusive Provider Organization.” This plan provides members with the opportunity to choose in-network providers within a broader network and to visit specialists without a referral from their primary care doctor. EPO plans offer a larger network than an HMO plan but typically do not have the out-of-network benefits of PPO plans. EPO plans do not require you to select a primary care physician (PCP) giving you a broader network of providers. EPO options are a great cost-saving option with more flexibility than a standard HMO plan. What is a PPO Plan? PPO stands for “Preferred Provider Organization.” PPO plans are often more flexible when it comes to choosing a doctor or a hospital. These plans still include a network of providers, but there are fewer restrictions on the providers you choose. PPO plans do not require you to select a primary care physician (PCP), giving you a broader network of providers. So, which plan should you choose? Each plan type has different benefits, so it depends on your health needs when choosing the right plan type. If you are looking for flexibility when choosing providers and locations, a PPO plan may better fit your needs. An EPO plan may be a better option if you want the flexibility of a larger network, but don’t necessarily need out-of-network benefits. If you regularly seek care in a certain geographic area and are looking for a health insurance plan at a lower price point, consider an HMO plan. To keep costs low, insurance carriers contract with providers and partner in plan members’ health to ensure quality care at the lowest cost. Whether you choose an HMO, EPO or PPO option, partnering with your health insurance carrier and your healthcare provider will help you receive the best care while controlling your out-of-pocket costs. Keep in mind that most insurance carriers offer emergency care coverage for all three plan options (HMO, PPO, EPO). Get the most out of your health insurance benefits! Established in 1988, Hometown Health is the insurance division of Renown Health and is northern Nevada’s largest and only locally-owned, not-for-profit insurance company providing wide-ranging medical coverage and great customer service to members.
Read More About Health Insurance Terms Explained: HMO, EPO and PPO Plans
-
Understanding the Risks of Colon Cancer
Colorectal cancer is the second-deadliest cancer in the United States – largely because it goes undiagnosed. Dr. Christi Matteoni, Division Chief of Gastroenterology at Renown Health, discusses the symptoms and key screenings used to detect this type of cancer, along with risk factors and lifestyle changes that could affect the likelihood of getting the disease. What are some of the signs and symptoms of colorectal cancer? Many cases go undiagnosed because polyps can develop and become cancerous without any symptoms. Additionally, since colorectal cancer begins as small polyps, symptoms usually aren’t seen until later stages. This is why screenings are especially important. For those who do experience symptoms, the signs are often tied to your bowel habits. This can include changes such as constipation or diarrhea, narrow or dark stool, rectal bleeding, abdominal cramping, weakness and fatigue or unintended weight loss. What are some of the risk factors associated with this type of cancer? There are risk factors that can and cannot be controlled. Uncontrollable factors include age, race, personal and family histories as well as certain genetic syndromes that are important to discuss with your provider. This type of cancer is more common in people over the age of 50, African Americans and those of eastern European Jewish (Ashkenazi) descent. This type of cancer is also more common in those who have been diagnosed with polyps, Crohn’s disease, ulcerative colitis and long-term inflammatory bowel disease. important to discuss any of these risk factors with your provider. There are also lifestyle factors that can help reduce your risk. Factors include being overweight, having a diet high in red and processed meat, as well as smoking and consuming excess alcohol. Conversely, diets high in fruits and vegetables and a regular exercise routine can help lower your risk. If someone has some of these risk factors, what should they do? Do they need to get tested? If you are 45 or older and have any of these risk factors, we recommend you speak with your primary care provider about a formal colorectal risk assessment. The most common form of screening is colonoscopy. This screening lets your doctor examine the length of your colon, map out any potential problem areas and remove polyps. For most people, colonoscopies are recommended every 10 years starting at age 50. However, depending on your results and risk factors, you may need to begin screening sooner or get screened more frequently. What do diagnosis and treatment look like for this type of cancer? There are several diagnostic options for colorectal cancer, including endoscopic ultrasound; CT, MRI and PET scans; and biopsy and pathology reports. These technologies allow your doctor to get images of your colon and evaluate what treatment is needed, as well as how the treatment is progressing. Treatment varies for each individual working with their doctor. In the case of colorectal cancer treatment, the William N. Pennington Institute for Cancer offers chemotherapy, radiation therapy, surgery and clinical trials.
-
Why Can't I Eat Before Surgery?
If you’re having surgery on your shoulder, why does it matter what’s in your stomach? We asked Dr. Matthew Hoberg to explain more about pre-surgery directives, including fasting. If you have an upcoming surgery, your care team likely gave you instructions to fast before your procedure. But why? We asked Matthew Hoberg, M.D., medical director of Renown Surgical Services, to explain why it’s important to forgo food and drinks before surgery. Why are patients instructed to fast before surgery? Regardless of surgery type or site, we want the stomach to be empty before having anesthesia, because anesthesia can reduce your body’s ability to protect and prevent food or acids from the stomach from entering the lungs. Normally, your body is able to prevent this, but anesthesia medicines make it harder for your body to do so. When food or liquids from the stomach get into the lungs, doctors call it “aspiration.” This is rare, but can be dangerous if it does happen. Solid foods and liquids leave the stomach at different rates too. Solid food takes longer to empty from the stomach than liquids, so the time to stop eating solids (eight hours) is longer than that for clear liquids (two hours). The body has energy reserves to produce needed nutrients and fuel during fasting. Recently, studies have shown it is important to stay hydrated and have some carbohydrates in clear liquids up to two hours before surgery, so clear liquids are allowed until two hours before surgery. There are also special rules for babies and young children who need surgery. For example, you may give breast milk up to four hours before surgery. If your baby drinks formula, you should stop six hours before surgery, and all solid foods you should stop eight hours before. Your child’s doctor or nurse will give you exact instructions. What if you show up for surgery and have broken the no-eating rule? Will surgery be re-scheduled? If patients have not followed the fasting guidelines, surgery will be postponed or rescheduled due to the possible increased risk associated with not having an empty stomach. The exception would be emergency surgery that cannot be delayed in which case special precautions are taken to help prevent anything from getting into the lungs. What other pre-operative rules should be followed to the letter? All instructions given to patients before their surgery or procedure should be followed. There are specific medical reasons behind all the instructions and they are designed for safety — to minimize risks, lower complications like infections and enhance the recovery process to help patients get back to normal as quickly as possible. Also, many patients ask if they should continue taking medications before surgery. The answer is: It depends. Your doctor or nurse will tell you which medicines you should take and when. Some medicines need to be stopped before surgery. But for others, it’s important you keep taking them as usual. You may also get new medicines to take before surgery. You may be asked to take some medications before surgery as part of advanced pain management protocols. If you need to take medicine right before your surgery, you can take it with a sip of water.
-
Want to Recover from Surgery Faster? Get Moving!
To be on the move is a scary concept when you’re recovering from surgery. But did you know getting up and at ’em could be the key to a quicker recovery, post-surgery? Here’s some expert insight from Renown Surgical Services. The team at has some news for you: Rest and movement are important to prevent serious complications. Here are some tips about how to get mobile after your procedure — and why it’s fundamentally important. Tip 1: Start Simple While you’re in bed, move your legs and feet up and down. Be sure to ask the nurses to help you get out of bed and into the chair for all your meals, or walk to the bathroom when needed. If you feel up to it, take a walk in the hallways with the nursing staff. Tip 2: The Sooner, the Better This may be surprising, but too much rest is not necessarily a good thing. The old saying “You use it, or you lose it” rings very true to maintaining the strength needed to get yourself out of bed. Beginning the mobility process early in your hospital stay will not only help you maintain strength and function, it may also help you get home sooner. Though it may seem counter intuitive, lying in bed all day can delay your healing time and cause serious complications to arise, including pneumonia, deep vein thrombosis or blood clots, pressure ulcers and sometimes constipation. Tip 3: Mobilize Your Support System Getting out of bed, sitting in a chair for meals and walking around your room or hospital unit can help reduce your risk of complications. The nursing staff will help you out of bed the same day of your surgery if it’s cleared by your doctor. Tip 4: Safety First The nursing staff is here to keep you safe, so make sure you call them for assistance getting out of bed. Even if you think you can do it yourself, use your call light to notify the nursing staff you are ready to get up and move. In addition, new medications can sometimes impair our judgment, balance and safety, so it’s always better to have help even though you may not need it. This is also why you may have a “bed alarm” on, to remind you to call for help and keep you safe while you are recovering. Tip 5: Move, But Manage Your Pain Many people find that getting up and moving actually helps their pain, rather than making it much worse. Taking the right amount of medication at the right times will minimize your pain and help you to get moving. Your care team will work with you on how much pain medication is right to manage any postoperative pain, with the goal for you to be comfortable enough to be able to move and gradually increase your activity each day. Tip 6: Maintain that Momentum at Home Mobility doesn’t end once you’re discharged from the hospital. It’s key to keep moving to maintain health and function. When you first arrive home, it’s crucial to take frequent movement breaks throughout the day. Increase activity as it becomes more comfortable, and be sure to ease back into an active daily routine. If you have concerns about your mobility once home, be sure to discuss this with your doctor at your follow-up appointment. Renown Surgical Services | 775-982-3993 Ask your doctor if you have any questions about your medical condition or the specific surgical procedure planned, or contact the team at Renown Surgical Services. Learn More
Read More About Want to Recover from Surgery Faster? Get Moving!
-
Got a Cough, Runny Nose, Sore Throat and Fever? It Might Be RSV Virus
Renown Urgent Care team prepares you to stay alert and safe this season and is available for medical assistance, 7 days a week at 11 locations across northern Nevada. In June, staffers at the Centers for Disease Control and Prevention sent a Health Advisory requesting that clinicians and caregivers watch for the respiratory syncytial virus, usually known as RSV, an infection that puts thousands of toddlers and senior citizens in the hospital each year with pneumonia and deep lung inflammation. According to the CDC, RSV results in roughly 58,000 hospitalizations and 100 to 500 deaths each year among children under five as well as 177,000 hospitalizations and 14,000 deaths among adults 65 and above. RSV was cropping up in 13 southern and southeastern states, the agency warned, and clinicians should test for the virus if kids showed up sneezing, wheezing, or with poor appetites and inflamed throats. Usually a winter infection, RSV is usually gone by June. Instead, this year, it is spreading—and has since continued to spread across the country, and to northern Nevada. “We know that many of the good hygiene habits we developed to defend against COVID-19 disrupted the viral landscape over the past 16 months, suppressing infections from almost every pathogen. Now RSV’s out-of-season return tells us that we need to continue to be on the alert,” says Robert Thole, MD, a physician with Renown Urgent Care. “We are surprised to be seeing so many kids with RSV right now.” “We ask parents and caregivers to keep a watchful eye out for a respiratory syncytial virus (RSV) infection. Symptoms are usually mild and resemble those of the common cold. RSV infection sometimes leads to bronchiolitis, pneumonia, or both. Symptoms of these complications include; difficulty breathing; wheezing; coughing that is getting worse; lethargy, increased tiredness, decreased interest in surroundings, or loss of interest in food,” explains Dr. Thole, who is board certified in family medicine. Catching and spreading the virus People with RSV infection may spread the virus through their secretions (saliva or mucus) when they cough, sneeze, or talk. You can catch the virus by: Touching an object or surface contaminated with the virus and then touching your nose, eyes, or mouth without first washing your hands. The virus can survive for more than 6 hours on countertops and other hard surfaces, such as doorknobs, and for 30 minutes on hands, clothing, or tissue. Close contact. If an infected person coughs or sneezes near you, you could breathe in RSV that is in his or her saliva or mucus. The virus spreads easily in crowded settings, such as childcare facilities, preschools, and nursing homes. Children attending school often spread the virus to their parents and siblings. The incubation period—the time from exposure to RSV until you have symptoms—ranges from two to 8 days but usually is 4 to 6 days. People are most likely to spread the virus within the first several days after symptoms of RSV infection begin and remain contagious for up to 8 days. Babies and young children may spread the virus for at least 3 to 4 weeks. Most children and adults feel better after a week or two. Treatment For an otherwise healthy child who has symptoms of an upper respiratory infection, such as a cough or runny nose, home treatment usually is all that is needed. It is important to watch for signs of complications, such as dehydration. Watchful waiting may not be a good choice when your child with an upper respiratory infection has an increased risk for complications. Watch your child closely if there are symptoms of an upper respiratory infection. If symptoms get worse or new symptoms develop, see a doctor right away. There is no vaccine and few specific treatments aside from supportive care, such as administering pain relievers and fluids. In the most severe cases, some children or adults might need additional oxygen. Not just in kids, older adults at risk Dr. Thole explains, “RSC is not only seen in children. Adults older than 65 have an increased risk of complications following infection with RSV. Pneumonia is a particular risk, especially if other health problems exist, such as chronic obstructive pulmonary disease (COPD) or heart failure. It may take older adults longer to recover from RSV infection and its complications than people in other age groups.” Call 911 or other emergency services immediately if: Your child has severe trouble breathing. Your child's breathing has stopped. Start rescue breathing. Call your doctor now if your baby or child has moderate trouble breathing. Call a doctor if your child: Breathes slightly faster than normal and seems to be getting worse. Most healthy children breathe less than 40 times a minute. Has cold symptoms that become severe. Has shallow coughing, which continues throughout the day and night. Has a poor appetite or is being less active than usual. Has any trouble breathing. Hospitalization Doctors sometimes give a monoclonal antibody treatment to high-risk babies throughout the respiratory season to prevent them from catching the virus or developing a severe infection. Some hospitals have started to increase use of the prophylaxis in response to the recent uptick in RSV cases. “Those kids were being protected,” said Kristina Deeter, MD who was quoted in a July 1st Wall St. Journal article on this topic. Dr. Deeter is a pediatric intensivist and medical director at Renown Children’s Hospital Pediatric Intensive Care and Hospitalist Medicine. Dr. Deeter, who also oversees Pediatrix Medical Group’s critical-care team in dozens of pediatric intensive care units across the country, said hospitals are also considering taking additional precautions in the neonatal intensive-care unit similar to some wintertime protocols. At Renown Children’s Hospital, there were no children hospitalized with RSV throughout the winter season, Dr. Deeter said, when there are normally hundreds of cases in our county- many of which do not need to be hospitalized.” A total of 31 cases have been reported in Washoe County, Nev., since April, and 26 of those occurred within the past three weeks. Preventing infection To prevent infection, or at least to mitigate them, wear masks, stay home when sick, and washing hands could make a difference in how the next viral season unfolds. For more information on RSV, visit renown.org. Renown Urgent Care Renown Urgent Care is available for medical assistance, 7 days a week at 11 locations across northern Nevada providing treatment for a wide range of minor injuries, illnesses and medical concerns that are urgent but not life-threatening. If you require same-day medical attention, you can avoid the long wait times and high prices of the emergency room at 13 convenient sites, including Reno, Sparks, Carson City, USA Parkway, Fallon and Fernley. You can walk-in or book ahead online. About Renown Health Renown Health is a locally governed, not-for-profit integrated healthcare network serving northern Nevada, Lake Tahoe and northeast California. Renown is one of the region’s largest private employers with a workforce of more than 7,000. It comprises three acute care hospitals, a rehabilitation hospital, the area’s most comprehensive medical group and urgent care network, and the region’s largest and only locally owned not-for-profit insurance company, Hometown Health. Renown has a long tradition and commitment to improve the care and the health of our community. For more information, visit renown.org.
Read More About Got a Cough, Runny Nose, Sore Throat and Fever? It Might Be RSV Virus
-
Why I Give: The Meinzer Family’s Story
Losing a loved one is a devastating experience that can leave a permanent mark on one's heart. It is a journey that's difficult to navigate, but with the help of family and friends the process can be eased. For the Meinzer family, the healing process was made a little easier because of the exceptional care their loved one, Susie, received at Renown. In the fall of 2022, Susie Meinzer, a breast cancer survivor, suffered a fatal stroke. The care provided by Renown’s team was a reminder of the important role healthcare workers play in the lives of their patients and families. “We just knew, the doctors, the nurses, everyone… we knew that we didn’t have much time left with Susie,” said Ken Meinzer, Susie’s widower. Humanizing Healthcare The compassion provided by the care team at Renown made a significant impact on the Meinzer family. They ensured that Susie's last moments were as comfortable as possible, and their kindness and empathy have stuck with the family since. Dr. William Graham, pulmonologist with Renown Health, was among the many healthcare workers who provided care to Susie. "It was hard enough to lose her, and we ask ourselves, ‘Why?’ a lot, but the compassion we received from Dr. Graham made it a little bit easier,” said Ken. “One night he sat with us for over an hour, just grieving with us." This act of kindness made a profound impact on the family. “As an ICU doctor, I try not only to care for my patients, but also for their families,” said Dr. Graham. “Ken and his family displayed such sincerity, compassion and love for Susie and one another. They are just wonderful people; the kind of people that inspire me to be the best doctor possible.” A Family Legacy In gratitude for the exceptional care Susie received, the Meinzer family, including Ken and his three daughters, Melissa, Nicole and Kyra, decided to donate to Renown Health Foundation. Their gift is a beautiful reflection of their love and devotion to Susie. “The donation was a way to say thank you, and a way to support the healthcare workers who continue to make a difference in the lives of patients and families every day,” said Ken. "The nurses in Renown’s ICU went above and beyond. They were a constant source of comfort and support for our entire family," said Melissa Meinzer-Benson, Ken and Susie’s eldest daughter. This was not the first time the family had experienced exceptional care at Renown. Ken and Susie had both undergone cancer treatment the previous year. Susie was diagnosed with breast cancer and had recently completed her treatment before her stroke, while Ken was treated for neck cancer. Dr. Abhinand Peddada, oncologist with Renown Health, led both their care teams, demonstrating a deep dedication to their well-being throughout their treatments. “I am grateful and humbled by the trust that Mr. and Mrs. Meinzer placed in Renown and me for their care in difficult times,” said Dr. Peddada.” Both Ken and Susie deeply appreciated Dr. Peddada’s care for them throughout their respective battles with cancer. The Meinzer family, who own Pinnacle Heating and Air Conditioning in Reno, are known for their commitment to giving back to the community. Melissa is a Veteran and has spoken about the importance of supporting others in any way possible. Susie instilled in Melissa and her sisters a spirit of compassion from an early age, and they have continued to donate to charitable causes throughout their lives. “She was such a force of inspiration, compassion and love. She was aways caring for others,” said Kyra, Ken and Susie’s youngest daughter. Susie was a beloved member of the Oak Community Church. It was there that she spent many Thanksgivings alongside her daughters, volunteering to serve meals to those in need. Charity work was a passion for Susie, and she always found ways to help those around her. She was a shining example of the importance of supporting your community and making a positive impact on the world.