Search
-
Make Hydration a Priority for Your Health
As the temperatures skyrocket and we return to more outdoor activity, one thing is certain: you must hydrate to stay cool, healthy, and functional. But how much water do you need, and what are some easy ways to ensure you are getting enough? Aurosis Reddy, DO a family medicine provider with Renown Medical Group, shares what you need to know. How Much Water Is Enough? Experts agree that recommended daily water intake can vary depending on different factors such as your weight, metabolism, location, diet, physical activity, and health. As a rule of thumb, women should aim for a daily fluid intake of 91 ounces, and men should aim for 125 ounces. It is important to listen to your body and recognize when you might need to increase your water intake. For example, if you’re partaking in strenuous exercise, or spending time outside in the heat, you’ll want to give your body more water and electrolytes to function properly. How Can I Tell If I Am Dehydrated? Decreased coordination Fatigue Less urination Dizziness Dry, sticky lips and mouth Increased thirst Headache
-
Three Things to Know About the Enhanced Benefits of Renown’s New Medicare Program
Renown Health recently announced that it has contracted with the Centers for Medicare and Medicaid Services (CMS) on a new program that offers enhanced Medicare benefits for Medicare beneficiaries. This new direct contracting Medicare program is designed specifically for patients with Original Medicare. Here are three things to know about Renown’s new program: The goal of the program is to help care providers work together to improve patients’ health by better coordinating patient care and reducing costs. Medicare beneficiaries who choose to sign up will have peace of mind knowing that they are in a program that ensures coordinated care along with potential cost-sharing assistance for chronic care management. Signing up for this program is easy – and it does not affect your existing Medicare benefits in any way. Simply click the button below, select either your current Renown Health or Geriatric Specialty Care provider from the drop down menu, complete the form and click “Submit Form.” It only takes a minute or two to fill out the form. You will be asked to provide the name of your primary care provider and be sure have your red, white, and blue Medicare card handy. Sign Up for Renown’s Enhanced Medicare Benefit Program Voluntary Alignment Sign Up Note: Participation in this program is voluntary. If you choose to sign up, your benefits will NOT change, and you can visit any doctor, other health care professional, or hospital. Learn more about Renown’s Direct Contracting Entity for Medicare Beneficiaries here. The statements contained in this document are solely those of the authors and do not necessarily reflect the views or policies of CMS. The authors assume responsibility for the accuracy and completeness of the information contained in this document.
Read More About Three Things to Know About the Enhanced Benefits of Renown’s New Medicare Program
-
Dorm Safety and Bacterial Meningitis
Bacterial meningitis is probably the last thing on your mind as you help your child prepare for college. Buying books and stocking up on necessities may top your list, but it’s a good idea to ensure your student is up-to-date on their meningitis vaccine. How Bacterial Meningitis Spreads According to the Centers for Disease Control and Prevention, people living in close quarters are more likely to spread this illness to one another. For example, you may have heard about the higher risk of meningococcal (or bacterial) meningitis for new college students. The risk is so serious that many colleges and universities require proof of a vaccine for new students moving into campus housing. This includes the University of Nevada, Reno. To clarify, all incoming freshmen under 23 years of age must show proof of their up-to-date meningitis shot. “Bacterial meningitis is considered a medical emergency, and anyone with the signs and symptoms should be evaluated in the emergency room immediately,” says Vanessa Slots, MD, Renown pediatrician. Symptoms of Bacterial Meningitis Fever Nausea Vomiting Irritability Headache Confusion Back pain Stiff or painful neck Leg pain Light sensitivity Rash on the torso or lower extremities It’s important to know many of these symptoms for both bacterial and viral meningitis are the same. However, the viral type is more common, often clearing up in seven to 10 days without complications. Nonetheless, you should go to the emergency room to be looked at, as the signs are similar for both illnesses. Why is Bacterial Meningitis Dangerous? This illness moves quickly, and in some cases, it can seem like the flu or severe strep throat and take a few days to develop. Or, it can hit in just hours. “Bacterial meningitis has an overall death rate of 10 to 15 percent despite treatment with antibiotics,” Dr. Slots warns. Another critical point is problems after recovery can also be severe. Frequently these include brain damage, amputations, infections around the heart, seizures and shock.
-
Dave's Story: How One Ranger Drove On
Meet Dave Pierson and his Wife Kathy Dave Pierson, 73, and his wife Kathy were just ten days away from a celebratory retirement trip to Africa in May 2021 when severe leg pain and discomfort landed Dave in the Veterans Administration (VA) Hospital. Unbeknownst to the couple, they would not be making the trek to Africa, and it would be several weeks before Dave would be back home with his wife in Carson City, their life drastically different than before. It all happened so fast. After a prompt referral from the VA Hospital to Renown Regional Medical Center, Dave received treatment for a bacteremia infection and underwent emergency spine surgery due to an epidural abscess. However, once his surgeon Edward Perry, MD completed the emergency procedure at Renown Health, Dave learned there was still a long road ahead. He had extremely limited body function and would need to learn to walk again. A Husband, Baseball Fan and Veteran Until this emergency spinal cord surgery, Dave had lived an especially healthy life in his retirement, traveling the world with Kathy, taking photographs along the way and attending ball games for their beloved team, the Reno Aces. Dave, a Vietnam veteran, and Kathy planted their roots in Carson City surrounded by countless friends and family, eagerly awaiting Kathy’s retirement. The Long Road Ahead It was those same friends and family who remained by Dave’s side throughout his recovery process. At the advice of the Renown team, Dave began a personalized physical rehabilitation plan at Renown Rehabilitation Hospital just days after his initial surgery. It was with the help of Charles Krasner, MD, an Infectious Disease Specialist that Dave made a smooth transition to be cared for at the Rehabilitation Hospital. Dave spent six weeks of inpatient treatment relearning fundamental occupational skills and motor functions such as eating and drinking, getting dressed, using a wheelchair and eventually taking his first steps, aided by a walker. The couple proudly remembers a day at the Rehabilitation Hospital when Dave successfully buttoned up his shirt using a small apparatus designed to aid in the task. "It was a little thing, but it was a monumental thing," Kathy shared. Dave achieved physical and cognitive victories, both on a small and large scale, over the next six weeks. Kathy visited every day she could, always prepared with a photo of the couple's past travels to encourage Dave. The Rehabilitation Hospital staff grew close with the Piersons, sharing stories and photos of their dogs, travels and life. The nurses kept Kathy updated about her husband’s condition and prepared her for the journey to come, this included extensive education related to Dave’s future at-home care. Benjamin Pence, MD, Dave’s lead rehabilitation doctor and the Director of the Institute for Neurosciences, always seemed to know just how to motivate Dave on his most challenging days. As a ranger in Vietnam, the phrase, “drive on ranger” meant a lot to the veteran when it came to determination and perseverance. So, the phrase was used as encouragement by Dr. Pence and the Rehabilitation Hospital team throughout Dave’s journey, becoming a fond memory about hope and determination during recovery.
-
Meet Gabby, Renown Regional ER Nurse and Miss Rodeo Nevada
Renown Health is proud to embrace the Reno-Sparks culture that makes our community stand out, which is why we sponsor the Reno Rodeo, an early summer staple with roots in the community as deep as our own. One of our many ties with the Reno Rodeo includes Renown Regional’s own emergency room nurse and Miss Rodeo Nevada 2022, Gabby Szachara. A Reno native, Gabby developed a love for the Reno Rodeo at a very young age. “I loved watching the girls on the Reno Rodeo Flag Team when I was little and knew I wanted to be part of the Reno Rodeo someday,” said Gabby. “As I got older, I started to make connections and build relationships with some people in the rodeo scene, and they generously lent me their horses so I could participate in the Reno Rodeo Flag Team.” Gabby was on the flag team for three years before being crowned Miss Rodeo Nevada 2022 last year. Before joining the Reno Rodeo Flag Team, Gabby was a student at the University of Nevada, Reno, and a member of the women’s volleyball team. In December 2017, she graduated with a bachelor’s degree in public health. At first, Gabby was interested in a career in sports medicine – it made sense with her background in athletics. But, after working in the medical field as a certified nurse assistant and an emergency medical technician, she grew passionate about patient care and decided she wanted to become a nurse. “I’ve always loved teamwork and helping others,” said Gabby. “It’s important to me to be there for others, especially when it might be their worst day.” In December 2021, Gabby graduated from Truckee Meadows Community College with a nursing degree and joined Renown Health this February. “I love Renown for various reasons. Everyone here is so nice and welcoming, and there is a great team dynamic,” said Gabby. “And I love that Renown’s main color is purple because that is my favorite!” When Gabby isn’t in her scrubs and caring for patients, she is in western wear and carrying out her duties as Miss Rodeo Nevada. “I do a lot of traveling across the country to attend other rodeos,” said Gabby. “I enjoy meeting so many wonderful people and experiencing the culture of different states.” Gabby’s main goals as Miss Rodeo Nevada are to promote the western way of life, agriculture, rodeo and community benefit. In addition, she visits local schools to talk with kids about how they can get involved in these areas and inspires them to turn their dreams into reality. Gabby has a special place in her heart for the Reno Rodeo. “Reno is my home, and the Reno Rodeo is the heart and soul of summer in northern Nevada. Everyone comes together and dusts off their boots to have fun and also contribute money to important causes in our community,” said Gabby. “I love the comradery, the friendly and healthy competition and the great people.” If you’re going to the Reno Rodeo this weekend, watch for Gabby and her horse, “Torque.” And if you see Gabby in the halls at Renown Regional, give her a high-five for all her hard work as a nurse and Miss Rodeo Nevada!
Read More About Meet Gabby, Renown Regional ER Nurse and Miss Rodeo Nevada
-
A Blood Test: What Valuable Clues It Tells Your Doctor
Blood. It can make you squeamish to think about it, yet every drop is vital to your health. In fact, a tiny vial of it can tell your doctor a wealth of information. We asked Benjamin Hansen, M.D., to explain what providers can learn from a blood test and why it’s important to get one as part of your annual checkup. CBC, the initials, sound innocent enough, right? In fact, when your favorite TV doctor orders a CBC, or complete blood count, it’s often the first step in getting an overall picture of your health. "It primarily measures white blood cells, red blood cells and platelets," explains Hansen. Although a blood test is one test you don’t have to study for, the measurements it takes can point to a host of information. What a Blood Test Says About Your Health White Blood Cell Count "The white blood cell count in your CBC helps us to determine the strength of your immune system," says Hansen. "It also helps us to determine the likelihood of infection because white blood cells fight off infection. Knowing the white blood cell count can also be helpful in patients with compromised immune systems, such as those on certain medicines or with conditions that impair immunity," he adds. White blood cells are made in your bone marrow and are alive only one to three days. Therefore, your body is constantly making them. Red Blood Cell Count "The red blood cells carry oxygen from your lungs throughout your body, while also carrying away waste. The hemoglobin (red blood cell protein) count is important because it helps us determine how well you're able to deliver oxygen from your lungs to the rest of your body," states Hansen. If these counts are low, you may have trouble breathing or experience fatigue. Red blood cells also grow in bone marrow, but they have a long lifespan – generally 100 to 120 days. Why Get a Blood Test? Although the CBC is just one type of blood test, according to the National Institutes of Health (NIH) there are a number of blood tests available that can help check for diseases and conditions such as: Heart disease Cancer Anemia (low iron) Diabetes High cholesterol Alcohol or Drug use disorder HIV/AIDS Additionally some tests show how well your kidneys, liver, heart and other organs are working. If you are taking a medication, a blood test can also let your provider know if it is helping you. What to Expect From a CBC Blood Test When you are not feeling well, it may take some detective work to figure out what is wrong and sometimes a CBC can be helpful. With this in mind, a lab order from your provider is needed to order a CBC blood test. Some blood tests require you to not eat food (fast) eight to 12 hours before the blood draw. Your provider will let you know the type of blood test(s) they are ordering for you. Usually it's important to drink plenty of water before your blood test, to make it easier to locate your veins. Generally a small sample of blood is taken from your arm vein and then sent to a lab for analysis. Discussing Your Results "A CBC can help your provider determine if there is an infection, your level of immunity, if you are anemic or if you are prone to bleeding," says Hansen. When to Get a Blood Test "A CBC is usually ordered for a specified purpose. If you think you might need a CBC, please call your provider. It's also important to see your provider regularly to keep an eye on your health. Many patients should see their provider at lease yearly," Hansen clarifies.
Read More About A Blood Test: What Valuable Clues It Tells Your Doctor
-
Game-Day Slow-Cooker Vegetarian Chili
Are you settling in to watch the big game? Prep this easy-to-make vegetarian chili with a handful of wholesome ingredients hours before game time, and you’ll be ready to enjoy some healthy and flavorful chili by kickoff.
-
5 Training Tips for an Epic Winter Season
Whether it’s cross-country or downhill skiing, snowboarding or snowshoeing, your off-season preparation is vital to an injury-free and healthy experience once the snow starts to fall. We’ve got you covered with expert tips that will make you the king or queen of the hill. Millions of skiers and snowboarders hit the slopes annually. So whether you’re a weekend warrior or stay active year-round, you need to prepare your body for the demands of your favorite winter sport to avoid minor aches, pains or even severe injury. Count on two to three weeks for your body to adapt to the physical challenges ahead if you’re active. Otherwise, give yourself a minimum of six weeks to gear up for the snow. Ready to shred? Here are some conditioning tips to help put you on the path to a fun, successful winter season. 1. Start With Cardio Cardiovascular exercise increases endurance as it conditions the heart, lungs and muscles and provides a solid foundation for other forms of exercise. And when you live and play at altitude, you need even more endurance. “Research shows that our maximum heart rate, cardiac output and ability to exercise are suppressed at altitudes over 5,000 feet,” explains Daniel Staffa, PT, DPT, OCS, of Renown Rehabilitation Hospital. “In the Reno-Tahoe area, altitudes can quickly rise over 8,000 feet when we exercise in the Sierras, so it’s critical to have cardiovascular fitness to avoid associated fatigue and decreased mental alertness on the slopes.” Try this: Pick an aerobic activity you enjoy — speed walking, running, hiking, biking or a cardio machine like the elliptical trainer. Build up to a minimum of 30 minutes, three days a week. 2. Increase Your Strength Your core works overtime to stabilize the body and absorb the shock of pivots and turns and variable snow conditions. Strengthen your core, lower back, hamstrings and calves and you’ll go a long way toward guarding against ligament tears and damage to other joint structures. Stronger muscles will also allow you to relax while maintaining control and making those quick adjustments that uneven terrain demands. Try this: Squats, wall sits and lunges. Work your core and lower and upper extremities with a variation of sit-ups, crunches, back extensions and planks. 3. Integrate Plyometrics Staffa explains that if your legs aren’t used to absorbing the impact of landing, severe injuries can occur. Preempt such trauma with plyometric exercises, or “explosive movements,” that simulate the movements of your favorite sport. You’ll develop greater power in your legs when you combine plyometrics with your strength training. Try this: Incorporate multi-directional drills — such as lateral jumps and forward and backward jumps — on variable surfaces like a trampoline, solid ground, or a box or step. Here’s a challenge for the more advanced: Stand in front of a bench or box (12 inches or so). Jump up and then immediately back down. Do this 10 to 30 seconds at a time, rest and repeat. Or get old school and bust out the jump rope. 4. Improve Your flexibility Flexibility is the ability to move joints through their entire range of motion, from a flexed to an extended position. Being flexible will allow you to pivot, twist and turn and navigate varying snow conditions with ease. You can increase your flexibility while maintaining bone alignment with stretching. Don’t forget to warm up and cool down. Try taking it easy the first 15 minutes of your day on the hill; try starting with a beginner’s run or walk to warm up and prepare your body. Do the same at the end of the day or go for a brisk walk to cool down. Stretching will help return muscles to their normal length. Try this: Dynamic stretches such as leg swings, arm swings and torso twists. Target your quads, hamstrings, calves, and lower back. 5. Fuel for the Hill Staffa suggests loading up on healthy complex carbohydrates the day before you go out and bring along your favorite protein snacks. Assess the slopes before making that first run — is the snow heavy, fresh or wet — and stay mindful of your fatigue level throughout the day. Don’t forget to hydrate and re-hydrate before, during and after exercise. And most important, have fun! Visit Renown Physical Therapy and Rehab for more information. Or call 775-982-5001 to consult with our sports and orthopedic experts who can help you develop an individualized training program in preparation for the winter season, including methods for overcoming previous injuries and limitations.
-
A Mocktail Recipe to Get Excited About
Whether you’re participating in Dry January or not, the first month of the year is the perfect time to experiment with mocktails. An alcohol-free version of your favorite after-work indulgence – like this peach cooler – can be a great way to live a healthier lifestyle because taking time off drinking doesn’t mean you have to stop enjoying exciting flavor combinations.
-
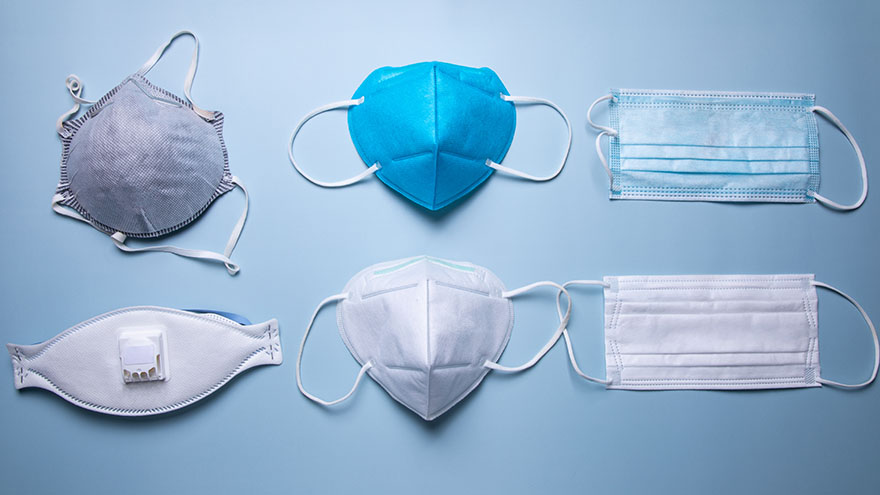
Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
To better protect our patients, visitors and employees, cloth masks are no longer allowed at Renown facilities. Surgical masks, KN95 and N95 masks are allowed at Renown facilities. Appropriate face masks will be provided for visitors and patients who need one. With recent surges in the infectious COVID-19 omicron variant, many have sought to upgrade their face masks. But, let’s face it, shopping for face masks with adequate protection can be a challenge, especially considering the countless variations and the rise of counterfeit masks. Follow our straightforward guide below which includes some common red flags to help you discern between a high-quality face mask that provides proper protection and those that may be counterfeit. Types of Masks Qualities of a Real N95 Respirator Mask According to the National Institute for Occupational Safety and Health (NIOSH), N95 approved masks form a tight seal around your face and include a disposable respirator that removes particles including bacteria, viruses and dust as you breathe. N95 masks that are NIOSH approved undergo strict quality assurance and performance requirements to ensure mask respirators filter out up to 95% of hazardous particles. As a rule of thumb, N95 masks will not have ear loops, commonly used in cloth or surgical face masks. N95 respirators will contain two elastic bands or head straps that fasten behind the head, one securing the crown of the head and the other resting at the base of the neck, providing a snug fit and seal. Some other common signs that an N95 might be counterfeit include lack of all proper labeling, misspellings of NIOSH, decorative fabric and claiming to be approved for children. Currently, masks in adult sizes are the only masks to undergo NIOSH’s quality assurance and testing process. Respirators approved by NIOSH will include a testing certification (TC) approval number and will contain specific labeling on the facepiece of your mask. Find a full list of Center for Disease Control (CDC) and NIOSH requirements here. Identifying Real KN95 Respirator Masks Often preferred due to comfortability, the KN95 respirators were initially designed to meet Chinese standards for medical masks. Firstly, if a KN95 mask claims to be approved by the CDC, it is counterfeit as the CDC and NIOSH do not support any respiratory protective devices according to international standards. However, when KN95 masks are fitted and worn appropriately they do provide more protection than disposable masks. Legitimate KN95 masks will display a manufacturer number, GB2626-2019, ensuring accordance with current Chinese respirator standards for all masks made after July 1, 2021. Unlike N95 masks, it is important to note that KN95 masks are available in children's sizes. You might run into KN95 masks claiming to be “FDA (Food and Drug Administration) approved” or “FDA-registered,” but be aware that this does not mean much and is a misleading statement. What this indicates is that a mask maker has submitted paperwork to the FDA, but the product has not been thoroughly tested for proper filtration and protection. Surgical Masks Medical procedure masks often referred to as surgical or disposable masks vary in their protection according to a variety of factors including fit and filtration. The CDC defines medical procedure masks as “variably shaped, including flat pleated, cone-shaped, or duck-bill. Medical procedure masks are loose and are not expected to provide a reliable level of protection against airborne or aerosolized particles as N95 respirators regulated by the National Institute of for Occupational Safety and Health.” However, these types of masks provide more protection than cloth masks and are certainly better than wearing no mask at all. Often popular due to their level of comfort and cost-effectiveness, surgical masks can be knotted in the ear loop areas to provide a tighter seal and can be layered for additional filtration. Depending upon your budget and level of comfortability and protection, one variation of mask may suit you over another. Please remember to do your part in limiting the spread of COVID-19 and wear a surgical mask, KN95 or N95 mask when visiting Renown facilities.
Read More About Avoid Counterfeits and Find the Right Protective Mask with This Helpful Guide
-
Club Member with a Grand Tale
Renown’s Sterling Silver Club is honored to feature one of our more than 9,000 members each season. We thank Judith for sharing her inspirational story and all of our members for leading healthy, happy lives that inspire us all. Mother, grandmother and eventually great-grandmother is the expected title progression as families grow and babies have babies. “Grand” and “great” usually imply roles and responsibilities have shifted from daily child-rearing duties to those of a doting grandparent – that is, unless you decide to do it all over again. At the age of 61, that’s exactly what featured Sterling Silver Club member, Judith, decided to do when she adopted four of her great-grandchildren. At the time, Alicia, Adrianna and Joey were all under five and Giancarlo, the youngest, was just a baby. “At the adoption hearing, the judge was concerned how stressful it would be for me to raise four children in my late 70s and early 80s,” recalls Judith. “But I told him I had raised my own four children and then three grandchildren for a number of years and that it would be far more stressful for me to have my great-grandchildren separated from each other and me, possibly forever. I knew I could handle the stress of raising them no matter my age, but I couldn’t survive the stress of losing them.” “That was when Giancarlo started getting fidgety,” she continues. “So I raised up his little shirt and blew a raspberry on his tummy which made him giggle and settle down. Seeing that, the judge told the recorder to “put that move in the record” and agreed I was capable of caring for my little ones.” Years later, Judith has come to realize that her great-grandchildren also want to be there to care for her. “Giancarlo always makes me smile,” says Judith. “Once during a stay in the hospital, I was awoken at 3 a.m. for blood work and found him sitting next to my bed watching the oxygen count – he was 10 years old at the time.” “The nurse asked him why he was awake and he said he heard her say the count shouldn’t go below 88, so he was watching to save me if it did,” Judith explains. “The nurse reassured him that she was also watching the count at her desk and he didn’t need to worry. Then Giancarlo looked her square in the eye and told her if it went below 88 to wake him up because he loved me and didn’t want to lose me.” “He is still my sunshine,” Judith smiles. “And I have never regretted my decision.” Work & Play For 20 years, Judith worked at Truckee Meadows Community College (TMCC), first as an administrative assistant for the police academy before moving to a position in the president’s office. There she worked with the TMCC Foundation and on TMCC projects to raise capital funds for new buildings, off-site campuses, scholarships, college programs and more. “It felt wonderful to be able to notify a student that they had received a scholarship or tell a department that they had received the funds to purchase needed equipment for their program,” recalls Judith. For fun these days, Judith still enjoys doing something she did as a teenager: playing pool. “My mother taught me to play pool in my dad’s pool room/teen hangout space in my early 20s and I’m just getting back into the game by taking lessons to help remind me what I was taught,” says Judith. “I grew up in a small, country town on the Ohio River and my mother could beat almost all of the boys in the county. I would love to be able to emulate her ability in the game.” Judith also enjoys reading, watching Hallmark movies or Warriors basketball games, walking in nature, playing “competitive” shuffleboard with friends, all genres of music – and dancing! In fact, she’s currently taking dance lessons to learn a few new steps. Always Good for a Laugh “My great-grandchildren and I laugh a lot when I try to teach them the stroll, twist, mashed potato and old-fashioned, rock-‘n’-roll dancing,” admits Judith. “But we laugh even harder when they try to teach me their dance moves!” Faith in What Matters Faith is something Judith celebrates and embraces for herself and others. “I truly believe that we are placed on earth exactly where God feels we are needed and that we are here to help each other through life, not to accumulate material goods for ourselves,” says Judith. “I feel deep satisfaction when I can help others either through just listening to them, advising them, helping them with specific needs or simply giving a smile to a stranger. To me, giving a smile or a helping hand to someone is like skipping a rock across the water – the ripples go on and on.” Then she adds, “And raising my great-grandchildren to be able to have wonderful lives full of love and happiness and closeness to God is the greatest gift I could give them.” Club Talk So what does Judith appreciate most about being a member of the Sterling Silver Club? She says it’s the opportunity to just – talk. “I fully enjoyed my initial interaction with the club and other club members at the Roaring Twenties dinner dance event,” remembers Judith. “I sat at a table with the nicest ladies and had great conversations with adults and danced with one of the instructors. When you are raising four teenagers who sometimes seem to speak an entirely different language, it’s refreshing to meet and speak with others your own age.” Pictures of some of the popular Sterling Silver Club events are featured here. Judith finds club events that bring her joy. “I also like the cooking classes and recently went on a walking tour of Oxbow Park, which was very peaceful.” What advice does Judith have to help other members live their best and fullest lives? “On a wet December morning 50 years ago,” Judith begins, “a truck coming around a curve on a country road slid into me and that split second could have made all the difference in the world to me. But God was with me and I survived, which no one expected.” “You never know when that one second that could change everything might happen, so make the most of all of your seconds,” she advises. “Do what you love with those you love. My family means the world to me and I try to think about how my decisions will reflect on the memory I will leave behind for them.” Then Judith thoughtfully adds, “I want them to remember that I truly loved them and always did my best to let them know that.”
-
Healthy Side Dish Cauliflower Rice
Finding the perfect cauliflower rice side dish can be challenging. Let's face it, not too many of us love the taste of cauliflower. However, this low-carb side dish is perfectly paired with chicken, rounding out a healthy meal. This recipe can also go well as a base to build a healthy and balanced protein bowl. Cauliflower Rice How-to Guide You can buy frozen riced cauliflower at just about any store, making it easy to throw into your recipes. However, if you want to make cauliflower rice yourself, here are some helpful tips to get you started. Registered dietitian Caitlin Bus hopes you'll give cauliflower rice a try as an alternative to traditional rice, allowing you to add more servings of vegetables into your diet!