Search
Results for 'primary care'
Clear-
Prostate Cancer: Symptoms, Treatments and Screenings
Did you know: More than 2.9 million men in the United States who have been diagnosed with prostate cancer at some point are still alive today. Prostate cancer is common, but also treatable, especially when caught early. Dr. Michael Hardacre of the Renown Institute for Cancer explains. With the exception of skin cancer, prostate cancer is the most commonly diagnosed form of cancer in American men. In fact, the American Cancer Society offers these key statistics: About 1 man in 9 will be diagnosed with prostate cancer during his lifetime. Prostate cancer develops mainly in older men and in African-American men. About 6 cases in 10 are diagnosed in men aged 65 or older, and it is rare before age 40. The average age at the time of diagnosis is about 66. The good news: This form of cancer is very treatable when also detected early. Michael Hardacre, MD, radiation oncologist with Renown Institute for Cancer, is here to explain more about prostate cancer screenings and their role in early detection. What is the prostate? The prostate is a gland that only males have, and it makes part of the seminal fluid. Prostate cancer begins when the cells in the prostate gland start growing uncontrollably due to a change in the cell’s genes. Researchers are working to find what leads to the disease. Certain types of prostate cancer are hereditary, or passed on through genes. However, most types of prostate cancer are acquired and developed later in life. What are some of the signs of prostate cancer? Common signs of prostate cancer include: Frequent urination Weak urine flow Painful urination or inability to urinate Blood in urine or semen Painful ejaculation Erectile dysfunction If you notice any of these signs, talk with your primary care doctor. Although it may be intimidating to talk about any of these signs or symptoms, the earlier prostate cancer is detected, the better the options for treatment. How can you screen for or detect prostate cancer? The good news is that prostate cancer can often be found before symptoms appear, because screening is as simple as a blood test. Your doctor will look for levels of a prostate-specific antigen in the blood. If the results come back with anything concerning, then additional testing would be recommended. A transrectal ultrasound can also be used, which is usually painless and only takes about 10 minutes to complete. This exam gives the doctor an image of the prostate to measure its size, which can help determine the density of the prostate-specific antigen. If this test comes back with any suspicious results, then your doctor may recommend a biopsy. What are the treatment options? Depending on each case, treatment options for men with prostate cancer might include: Watchful waiting or active surveillance Surgery Radiation therapy Cryotherapy (cryosurgery) Hormone therapy Chemotherapy Vaccine treatment Bone-directed treatment It’s important to discuss all of the treatment option with your doctors, including goals and possible side effects, to help make the decision that best fits your needs. Some important things to consider when choosing a treatment option also include: The stage and grade of your cancer Your age and also your expected life span Any other serious health conditions you have Your feelings (and your doctor’s opinion) about the need to treat the cancer right away The likelihood that treatment will cure your cancer (or help in some other way) Your feelings about the possible side effects from each treatment Renown Institute for Cancer | 775-982-4000 At the Renown Health Institute for Cancer, our experienced team provides the support and care to maintain the highest quality of life and then achieve the best possible outcome, all in one location that’s close to home. Our dedicated team, clinical expertise and also advanced treatment options allow us to tailor care to each patient. Learn about: Our Team Cancers We Treat Screening and Prevention Treatment Options
Read More About Prostate Cancer: Symptoms, Treatments and Screenings
-
Know Your Numbers, Save Your Heart
There are some important numbers to know when it comes to good health. Learn more and receive a free blood pressure check at a primary care open house Feb. 27 at Renown Medical Group – Double R. Know Your Numbers Adults are pretty good at knowing and memorizing numbers — from passwords and PINs to addresses and phone numbers. But what about the numbers that could help save your life? Heart disease remains the leading cause of death in the U.S., with 633,842 deaths attributed to the disease in 2016, according to the National Center for Health Statistics. The American Heart Association lists the vital numbers you need to monitor to help prevent heart disease as blood pressure, total cholesterol, blood sugar and body mass index (BMI). With these numbers, your doctor can assess your risk of developing heart issues such as atherosclerosis, which can lead to other serious heart conditions. Atherosclerosis is a condition wherein plaque builds up in the arteries — the blood vessels that transport oxygen-rich blood to cells, the heart and other organs. These fatty deposits clog the arteries, inhibiting blood flow and reducing the amount of much-needed oxygen the body receives. These blockages can lead to angina, coronary heart disease, peripheral artery disease and even heart attack or stroke. But knowing your numbers and keeping them in healthy ranges can mitigate your risk of atherosclerosis and other heart conditions. First things first: Make an appointment with your healthcare provider to see how you’re doing. Learn your numbers and discuss how they may increase your personal risk of heart disease: Total Cholesterol Because cholesterol contributes to the buildup of plaque, keeping your numbers in check means keeping your arteries free of blockages. Check LDL (bad) cholesterol and HDL (good) cholesterol. Your body needs low levels of LDL, but not enough good cholesterol in your system can also increase risk. You can maintain healthy numbers by staying physically active and consuming a heart-healthy diet low in cholesterol and sodium. Statins, the class of drugs used to reduce LDL cholesterol, have proven so effective that the U.S. Preventive Service Task Force recommended in November that all adults older than 40 with one or more risk factors consider taking them. Blood Pressure High blood pressure places undue strain on your heart and arteries to move blood and oxygen throughout the body. And a heart that’s working too hard can lead to stroke, heart attack and heart failure. High blood pressure cannot be cured, but it can be managed by eating a heart-healthy diet low in alcohol, staying active and maintaining a healthy weight. Blood sugar Given that the body converts most of the food we eat into glucose, or blood sugar, for energy, adding sugar to the diet can raise blood sugar to unhealthy levels and damage the heart, increasing risk of cardiovascular disease and obesity. Opt for foods that are low in fat and added sugars and, instead, get your sweets in naturally occurring foods. Let added sugars be a treat and not the norm. Body Mass Index (BMI) Your BMI is used to determine whether you’re at a healthy weight. If you’re carrying extra pounds, the heart has to work harder, which increases risk of heart disease. Losing those pounds and maintaining a healthy weight reduces the burden on your heart and blood vessels and improves your blood pressure and cholesterol levels. So eat a heart-healthy diet and get active — even if you simply walk for 30 minutes a day. Because no symptoms indicate that you have poor cholesterol numbers, high blood pressure or high blood sugar levels, getting screened and learning your numbers is vital. Your doctor can determine what healthy levels look like for you individually and work with you to develop a plan for staying in optimum ranges. That plan will include heart-healthy eating, exercise, abstaining from smoking and, in some cases, medication. It’s up to you to stick with that plan between doctor visits. Do it for yourself, but consider making a pact for a more heart-healthy, active life with a buddy. Research shows people stick with exercise plans longer when they have a partner. This article also appeared in the Reno Gazette-Journal’s Health Source Aug. 27.
-
Ask the Expert: What is Scoliosis?
Posture is important, but for those children diagnosed with scoliosis (spinal curvature) it can be a difficult issue. The Washoe County School District Student Health Services Department screens 7th grade students for scoliosis as growth spurts often reveal the condition and, if diagnosed early, scoliosis can stop progressing. We asked Michael Elliott, MD, head of the Department of Pediatric Orthopedics and Scoliosis to answer some frequently asked questions about scoliosis. What is scoliosis? There are many types of scoliosis: early onset (occurs before age 10), congenital scoliosis is when the bones of the spine do not form correctly, neuromuscular scoliosis which is due to children’s neurologic and muscle disease, and the most common is Adolescent Idiopathic Scoliosis. The term “idiopathic “ means the exact cause is unknown, although we do know it runs in families. This type of scoliosis occurs in 2-3 percent of adolescents and is mainly seen during their growth spurt. This is why middle school screenings are recommended. Both genders get scoliosis but girls are 8 times more likely to have their curves progress and become larger. What are the signs that my child may have scoliosis? A few signs for parents to watch for are: One shoulder might be higher than the other. One leg may seem longer. A hip may be higher or look more prominent. The waist may not look the same from side to side (asymmetry). The trunk or rib cage may be more prominent on one side or shifted. When they bend forward they may have a bump on their back. How is scoliosis diagnosed? It can be noticed by a pediatrician at a physical, school screening nurse, PE teacher or parents. Once the curve is suspected the child is usually referred to a pediatric orthopedic surgeon scoliosis expertise. At the initial visit the doctor will perform a thorough physical including a complete neurologic exam to assess the amount of curvature. Once the exam is completed the physician will determine if a spinal x-ray is needed. The curve on the x-ray is measured utilizing the cobb angle (a measurement in degrees) which helps guide the treatment. What are common treatments for scoliosis? The treatment depends on the size of the spinal curve and the amount of growth the child has remaining. An x-ray of the child’s hand is used to determine the amount of growth remaining. This allows the determination of the child’s bone age, and based on the hands growth plates it can determined if the child is in their rapid phase of growth. Treatments include: Observation - For curves less than 20-25 degrees. This entails visits every 6-9 months with a repeat scoliosis x-ray. Since scoliosis curves increase only 1-2 degrees per month, and variations in measurements can be 3-5 degrees, an x-ray is not recommended before 6 months. If the curve remains less than 25 degrees the child is followed until their growth is completed (usually age 16-18). Progressing Curve - If growth is finished and the curve is less than 40 degrees, the risk of more curvature into adulthood is small. If growth is completed and the curve is over 45 degrees, the child is followed for several years as these curves can progress into adulthood. If the patient is still growing and the curve has progressed greater than 25 degrees but still in the non-operative range (less than 45-50 degrees) bracing is used to stop the progression of the curve. Bracing - Indicated for curves over 25 degrees but less than 45 degrees. If a brace is required you will be referred to an orthotist (bracing specialist). The orthotist assesses your child, reviews the x-ray and then fits the brace. (Having a brace made usually takes 2-3 weeks.) Once the brace is fit, your child will visit the scoliosis specialist for an x-ray in the brace to ensure it fits correctly. The primary goal of bracing is to halt progression of the curve and prevent the need for surgery. The brace must be worn for about 16 hours per day to be effective. In a recent bracing study 72% of the patients who wore their braces as prescribed prevented the need for surgery compared to the group who did not wear their brace. Surgery: When a curve reaches 45-50 degrees, and a child is still growing, surgery is usually recommended because the curve is likely to continue progress. If a curve is over 50 degrees and the child is done growing surgery also may be recommended. This is because when curves are over 50 degrees they tend to increase 1-2 degrees per year for the rest of your life. As curves get larger the amount of lung function tends to decrease which could cause breathing problems later in life. The goals of surgery are to stop the progression of the curve and safely correct any misalignment. This is accomplished by attaching implants (rods, screws, hooks and bands) to the spine. Bone graft is then placed around the implants to encourage the spine to fuse (grow together). This then forms a solid column of bone with metal rods in place, preventing the curve from changing. Most patients are back to their regular sports and activities six months post surgery.
-
Cancer Clinical Trials and Research
The William N. Pennington Cancer Institute is dedicated to find the causes of cancer and develop better treatments. We research a wide variety of areas. We perform traditional research in the laboratory and translational research with patients, and we look at how we provide counseling and support and clinical trials, in which patients have the option to try new therapies. We partner with research institutions, including local researchers at the University of Nevada Reno (UNR) and the Desert Research Institute (DRI), national and international researchers, non-profit organizations, and industry to help drive discoveries forward quickly. Cancer Clinical Trials & Research Participating in cancer clinical trials and research allows you to receive the most effective therapy available. These treatments investigate promising new drugs, drug combinations, advances in personalized care, and new approaches to surgery or radiation therapy otherwise unavailable. To join a clinical trial, talk to a member of your cancer care team. They will know about any current trials for your type of cancer, explain your role in the preparation, and provide information about your protection. Trial participants usually receive the therapy at little or no cost. If you are considering a trial, consult with your primary care doctor. At William N. Pennington Cancer Institute, we want to provide our patients with the opportunity to access novel treatments through participation in clinical trials. For adult patients, we offer clinical trials through the National Cancer Institute Community Oncology Research Program (NCORP). Dr. Garrett Green, Renown Health department of Radiation Oncology, serves as the Principal Investigator and Liaison for the adult oncology team. For specific information on which trials are currently available at our institution, please call us at 775-982-5050. For children, we offer clinical trials including phase 2 and phase 3 studies through the Children's Oncology Group. Dr. J. Martin Johnston, Chief of Pediatric Hematology/Oncology at Renown Children's Hospital and Senior Investigator, Renown Institute for Cancer, is the Principal Investigator. The Cancer Research Team As the most extensive healthcare system in northern Nevada and eastern California, and in partnership with clinical trial sponsors, the National Cancer Institute, and the Nevada Cancer Research Foundation, we can access dozens of open clinical trials. We are here to provide education and guidance in making decisions about your care and treatment. Our specially trained research teams will help you understand the process and explain what to expect with each visit. We are committed to bringing the highest quality of cancer care to you and your loved ones. To learn more about open clinical trials, please reach out to us with this form.
-
Study From UNR Med and Renown in JAMA Network Open Highlights Gaps in Genetic Screening for Hereditary Breast and Ovarian Cancer
Data demonstrates that a proactive approach to family history assessment and genetic screening will increase early detection of inherited risk. A new original investigation article published in JAMA Network Open, “Screening Familial Risk for Hereditary Breast and Ovarian Cancer,” by authors from University of Nevada, Reno School of Medicine, Renown Health and Helix for the Healthy Nevada Project® emphasizes the critical need to increase genetic screening in identifying individuals at increased risk of breast and ovarian cancer due to family history. This landmark study calls for enhanced awareness, the adoption of genetic screening practices, and, importantly, the direct screening of family history by individuals using a simple tool such as the FHS-7 questionnaire. Breast and ovarian cancers remain leading causes of cancer-related deaths, with genetic factors playing a key role in up to 10% of cases. The study authors advocate for wider adoption of screening protocols, simple family risk questionnaires and education about the benefits of genetic testing, not only for patients but also their family members who may share similar genetic risks. Breast cancer is a leading cause of cancer death among women in the United States. According to the American Cancer Society, about 1 in 8 women will develop breast cancer and about 1 in 36 women will die from breast cancer. Since 1990, breast cancer death rates have declined progressively due to advancements in screening, treatment and detection. Here in Washoe County, Nev., the age-adjusted mortality rate for 2020 (last update) is 21 deaths/100,000 females due to breast cancer, which is higher and worse than the national U.S. value of 19.6. Nevada ranks near the bottom in breast and cervical cancer deaths in women according to a recent Commonwealth Fund report. Across the U.S., approximately 1.1 percent of women will be diagnosed with ovarian cancer at some point during their lifetime. The research underscores that individuals with a family history of breast and ovarian cancer have a higher likelihood of carrying genetic mutations in genes such as BRCA1 and BRCA2, which significantly elevate their cancer risk. However, many at-risk individuals remain unaware of their genetic predispositions due to limited screening practices. Evidence suggests that “up to 80% of patients with a pathogenic or likely pathogenic (P/LP) variant in the BRCA1 and BRCA2 genes are unaware of their condition and subsequent risk for hereditary breast and ovarian cancer. Rare or less penetrant P/LP variants in genes such as PALB2, CHEK2 and ATM are even less likely to be detected. This is concerning because the lifetime risk for breast cancer exceeds 50% for women with P/LP variants in BRCA1/2 and 20% for women in P/LP variants in PALB2, CHEK2 and ATM (compared with a baseline risk of 12%).” The study also found that men with family history are just as likely to have pathogenic variants in BRCA1 and BRCA2 as women. This is important because not only are men at increased risk of breast, prostate and other cancers, these risks are passed on to daughters, nieces and other members of the family through inheritance. Men are under-represented in the Healthy Nevada Project® and other similar population health studies. Daniel Kiser, MS, lead author of the study stated, "Our work shows that family history collected during routine medical care can be evaluated using simple criteria and used to identify patients with elevated risk for inherited cancers. Because there are a number of steps that can be taken to reduce risk, both for the patient and for their family members, following up with these patients has the potential to substantially reduce mortality and the incidence of cancer." “Prevention or early detection of disease is such an important part of healthcare,” says Bill Plauth, MD, MMM, CPE, Chief Medical Officer for Renown Health and Associate Dean for Clinical Affairs at the University of Nevada, Reno School of Medicine. “The Healthy Nevada Project® is leading the way in helping Renown Health physicians and clinicians assess family history risk of breast and ovarian cancer syndrome. This in turn, enables us to provide our at-risk patients the best available tools for prevention or to catch cancer at an earlier stage, which affords less aggressive treatment options with significantly improved survival.” The study found that routine genetic screening for individuals with a strong family history of these cancers could lead to more personalized and effective healthcare strategies, including preventative surgeries, increased surveillance, or early interventions. It also highlights the gap in awareness and access to genetic testing, particularly in underserved populations. “One of the lessons from our work is the importance of assessing family history early and often in the healthcare journey of patients,” says Joseph Grzymski, PhD, Chief Genomics Officer of Renown Health, the Principal Investigator of the Healthy Nevada Project, and a faculty member in the Department of Internal Medicine at the University of Nevada, Reno School of Medicine. “We recommend that everyone get screened for CDC Tier 1 conditions but particularly, when family history indicates risks, genetic screening is a powerful tool for risk stratification.” Key Recommendations from the Study Authors Include: Increased Engagement of Patients with Physicians: People with a family history should discuss their history with their primary care physician or health care provider and request a genetic screening. This proactive approach to prevention will save lives. Increased Access to Genetic Testing: The need for more accessible and affordable testing options, like the no-cost screening provided by the Healthy Nevada Project®, particularly for those with a family history of breast or ovarian cancer. Increased Pre-Screening and Genetic Counseling: Providing patients with the necessary counseling to understand the implications of genetic mutations and guide their healthcare decisions. Pre-screening patients with either a personal or family history of cancer with one of several simple family history tools, such as the FHS-7 Questionnaire to determine whether they should be referred for genetic services would also help increase early identification and reduce costs. As of January 2024, the Healthy Nevada Project® had notified 330 individuals with P/LP variants in BRCA1 or BRCA2 genes of their genetic risk, of a study population of more than 53,000 patients. The Healthy Nevada Project®, powered by Renown Health and University of Nevada, Reno School of Medicine, is one of the largest genomic studies in the United States. The genomic study is at no-cost for Nevadans and gives participants insight into different genetic traits, as well as results on their predisposition for three prevalent and serious health conditions known as the CDC Tier 1 conditions because of their significant potential to positively impact public health. Study authors include University of Nevada, Reno School of Medicine, (Daniel Kiser, MS; Gai Elhanhan, MD Iva Neveux, MS; William J. Metcalf, MS; Catherine McCarthy, MD; Leslie A. Greenberg, MD; Joseph J. Grzymski PhD); Helix, Inc. San Mateo, CA (Alexandre Bolze, PhD; Elizabeth T. Cirulli, PhD) and Renown Health, Reno (Savanna Grime, BA; Jamie M. Schnell Blitstein, APRN; William Plauth MD; Joseph J. Grzymski PhD. For more information on the study, please visit JAMA Network. For a media interview, please contact Dr. Joe Grzymski at news@renown.org. The Healthy Nevada Project®, led by Renown Institute for Health Innovation (Renown IHI) was launched in September 2016 as one of the first community-based population health studies in the United States. The study has already enrolled, consented and collected DNA from approximately 53,000 participants. Under the program, researchers and physicians are using genetics, environmental data and individual health information to empower providers with a targeted approach to personal health care and treatment, in turn improving the overall health and well-being of people in the local communities. The University of Nevada, Reno School of Medicine, Nevada’s first public medical school, is a community-based, research-intensive medical school with a statewide vision for a healthy Nevada. Since 1969, UNR Med has trained more than 3,900 students, residents, and fellows. UNR Med continues to improve the health and well-being of all Nevadans and their communities through excellence in student education, postgraduate training and clinical care, research with local, national, and global impact and a culture of diversity and inclusion. For more information, visit med.unr.edu. Renown Health is the region’s largest, locally governed, not-for-profit integrated healthcare network serving Nevada, Lake Tahoe, and northeast California. With a diverse workforce of more than 7,500 employees, Renown has fostered a longstanding culture of excellence, determination, and innovation. The organization comprises a trauma center, two acute care hospitals, a children’s hospital, a rehabilitation hospital, a medical group and urgent care network, and the locally owned not-for-profit insurance company, Hometown Health. For more information, visit renown.org.
-
Research Shows Genetic Approaches to Breast Cancer Screenings Yield More Accurate Results
Clinical researchers with the Healthy Nevada Project co-author research paper with findings that emphasize the need for a comprehensive approach to breast cancer risk assessment – including a focus on genetic medicine – to help ensure that individuals at high risk are identified and supported proactively rather than reactively. Breast cancer is a leading cause of cancer death among women in the United States. According to the American Cancer Society, about 1 in 8 women will develop breast cancer and about 1 in 39 women will die from breast cancer. Breast cancer is associated with increased age, hereditary factors, obesity, and alcohol use. Since 1990, breast cancer death rates have declined progressively due to advancements in treatment and detection. In Nevada there are an estimated 2,310 new breast cancer cases a year, and genetic mutations such as in the genes BRCA1 or BRCA2 remain a top risk factor for this prevalent disease. Recognizing the urgency for progress in breast cancer research, a collaborative effort between physicians, advanced practice providers and scientists from the Healthy Nevada Project® (HNP) and Helix have unveiled groundbreaking research. This study explores how genetic screenings are a necessary supplement to traditional testing methods, together offering more accurate insights into a patient's likelihood of developing breast cancer in the future. HNP is operated by Renown Genomic Medicine and the Institute for Health Innovation and is one of the largest community-based population health studies in the country. Their team works in collaboration with Helix, a leader in precision health that delivers comprehensive genomic solutions. Together, this dynamic partnership aims to understand breast cancer risk factors and pave the way for more effective preventative measures. The combined research team studied 25,591 female HNP participants to evaluate the performance of different genetic screening approaches to identify women at high risk of breast cancer. The results of this research suggest that a combined monogenic, or single-gene, and polygenic, or multi-gene, approach to breast cancer screenings helped produce more accurate results and more closely identify study participants who have a high genetic risk of developing the disease. "Based on this research, we are advocating a shift in approach which would improve breast cancer risk assessment through a combination of effective family history ascertainment and genetic screening,” said Joseph Grzymski, PhD, principal investigator of the Healthy Nevada Project, research professor at the University of Nevada, Reno School of Medicine and co-author of the breast cancer research paper. “This tailored approach, founded on the assessment of individual genetic risk, not only intends to elevate patient well-being but also will improve efficiency and equity in healthcare." Complementing the team’s research on leveraging genetics to identify women at low genetic risk of breast cancer that could safely defer mammogram screenings by five to 10 years that was released in late 2023 in JAMA Oncology, the study suggests that incorporating genetic information can assist in personalizing breast cancer screenings and optimizing the use of screening resources. "Existing disparities persist across various facets of breast cancer screening and treatment; however, genetic screening is clearly a powerful tool to help facilitate early intervention for those at higher risk,” said Jamie Schnell Blitstein, APRN, a primary care nurse practitioner at Renown Health and co-author of the breast cancer research paper. “By placing a heightened focus on risk, we underscore the pivotal role of preventative breast cancer screening.” Despite the availability of effective methods for early screening, co-authors of this research found that 78 percent of women with a family history of breast cancer had their risk ascertained only after a breast cancer diagnosis. The findings emphasize the need for a comprehensive approach to breast cancer risk assessment – including a focus on genetic medicine – to help ensure that individuals at high risk are identified and supported proactively rather than reactively. “These findings that can profoundly impact how healthcare is delivered were only made possible by all the participants who were willing to consent to research,” said Alex Bolze, PhD from Helix and co-author of the publication. “Broad-scale collaboration projects like these between Renown Health and UNR that engage large populations where participants share both their genetic information as well as electronic health records drive advancements in preventative medicine, as well as fundamental biological research.” The research paper was officially accepted on Jan. 29, 2024, and will be published by Elsevier, Inc. on behalf of the American College of Medical Genetics and Genomics. The contents of the paper will appear in the international journal Genetics in Medicine Open. Read the full article by visiting sciencedirect.com. The Healthy Nevada Project is currently recruiting new study participants. Free to all Nevadans with a saliva sample or blood draw, participants and their referring providers receive access to whole-exome sequencing and clinical grade results that help provide insight into their unique genetic risks tied to heart disease and certain cancers. If you are interested in enrolling in the study, schedule a Virtual Consent Appointment through MyChart or contact the Renown Institute for Health Innovation at RenownIHI@renown.org or (775) 982-6914 to be connected to a Genomic Representative. About Renown Health Renown Health is the region’s largest, not-for-profit integrated healthcare network serving Nevada, Lake Tahoe and northeast California. With a diverse workforce of more than 7,000 employees, Renown has fostered a longstanding culture of excellence, determination and innovation. The organization comprises a trauma center, two acute care hospitals, a children’s hospital, a rehabilitation hospital, a medical group and urgent care network, and the region’s largest, locally owned not-for-profit insurance company, Hometown Health. Renown is currently enrolling participants in the largest community-based genetic population health study, the Healthy Nevada Project®. To join the Renown Health team, visit renown.org/careers. About Helix Helix is the leading population genomics and viral surveillance company operating at the intersection of clinical care, research, and data analytics. Helix enables health systems, life sciences companies, payers, and government partners to accelerate the integration of genomic data into patient care and public health decision-making. Learn more at helix.com.
-
MD, APRN or PA: What's the Difference
Having a primary care provider is important and some health insurance plans even require you to select one. But does that provider need to be a doctor (MD)? The good news is your primary care provider doesn’t need to be an MD. They can be an advanced nurse practitioner (APRN) or physician assistant (PA). We’re here to explain the differences between MDs, APRNs and PAs. Have you ever called Renown Health to schedule an appointment with your doctor and the Contact Center offered you an earlier appointment with an APRN or PA? Did you wonder why? Perhaps you even declined because you were concerned about the continuity of your care, or wondered about the qualifications of the other practitioners who aren’t doctors. We’re here to answer your important questions about primary care providers and the different types. Why would I want to see anyone other than a doctor? In order to keep up with demand for primary care services and provide the highest quality care possible, Renown created care teams. This means our doctors, APRNs and PAs all work hand-in-hand to manage your health with the benefit of their combined expertise. This team approach provides you with more flexible scheduling options to see anyone on the care team, all with the same continuity of care. How qualified are APRNs and PAs to treat patients? APRNs and PAs are highly educated in medicine with a minimum of a Master of Science degree and at least six years post-high school education. Some APRNs even have doctorate degrees. Similar to doctors, both positions have a minimum number of required clinic hours and participate in continued education. Both APRNs and Pas are just as qualified as doctors (MDs and DOs) to conduct physical exams, diagnose and treat illnesses, order and interpret tests, write prescriptions and even deliver babies. There are some instances where you need a doctor, including specialized treatment of complicated or high risk conditions or surgery. Your APRN or PA will refer you to a doctor in those instances. You don’t need to worry about whom to see when – your care team will guide you based on your medical needs. If I see an APRN or PA, will my doctor know about my visit? Absolutely. The care team system ensures that everyone on your care team is aware of the details of your visit, regardless of who you’re seeing. Everything is clearly documented in your medical record so there are no gaps in care between visits. Can an APRN or PA be my primary care provider? Definitely. APRNs and PAs make excellent primary care providers and can be established with your insurance company. Learn more about the differences between doctors, APRNs, PAs and more with this handy infographic. Schedule A Doctor Visit | 775-982-5000 Renown Medical Group primary care providers provide annual exams by appointment. Our providers coordinate each patient’s medical care including checkups, immunizations, referrals to specialists, lab work, X-ray & imaging and hospital admissions. Request an Appointment
-
A Fighting Chance at 24 Weeks Sloans Story
Most babies weigh just one pound and are roughly the size of an eggplant when they reach 24 weeks of development inside the womb. It is a crucial stage when internal organs begin functioning, and the babies' respiratory and central nervous systems are still developing. So, in November 2021 when Kallie Johnson experienced a premature rupture of amniotic fluid around this point in her pregnancy, her care team in Winnemucca decided to transport her via Care Flight to Renown Regional Medical Center. The team at Renown Children’s Hospital immediately began discussing the risks of delivering at 24 weeks with the Johnson family. Moving Forward with Hope Knowing the stakes, Kallie remembers never feeling rushed to decide about delivering her baby preterm. “I felt educated and supported by my care team at Renown throughout our entire stay, starting with the education they provided about what it meant to deliver my baby early,” Kallie said. “The team really helped me make the best decision for myself and my family.” Together, Renown employees and the Johnson family moved forward with a healthy set of nerves and a powerful feeling of hope. Weighing in at one pound 11 ounces, Sloan entered the world on Nov. 19, 2021, via emergency Cesarean section. Her birth was classified as a micro preemie because she was born before week 26 of pregnancy and so small that she fit inside the palm of her father Sterling’s hand. A full-term pregnancy is classified as reaching 39 weeks. A Fighting Chance Called a fighter by many Renown Children’s Hospital care team members, Sloan spent over five months in the neonatal intensive care unit (NICU). She was placed on a ventilator, fed through a feeding tube and monitored 24/7, overcoming daily challenges with the Renown team and her family. As a result of being born prematurely, Sloan developed a grade one brain bleed and a congenital heart defect called patent ductus arteriosus, a persistent opening between two major blood vessels, causing too much blood to flow to the lungs and heart. To meet the oxygen needs of her tiny lungs, Sloan was intubated and developed a severe oral aversion and high-arched palate as a result. The effects would lead to difficult developmental and physical challenges that she still conquers today. Yet, with the help of her care team – including physical, occupational and speech therapists, dieticians and doctors – Sloan continues to make progress every day.
-
Stroke Program
Stroke is the 5th leading cause of death in the U.S. and the main cause of adult disability. If you or a loved one is experiencing a stroke, you need skilled medical care immediately. The Renown Neurovascular and Stroke Program provides expert emergency stroke care and comprehensive neurovascular care and rehabilitation services. If you suspect that you, or someone around you, is having a stroke, don't hesitate and call 911 immediately.
-
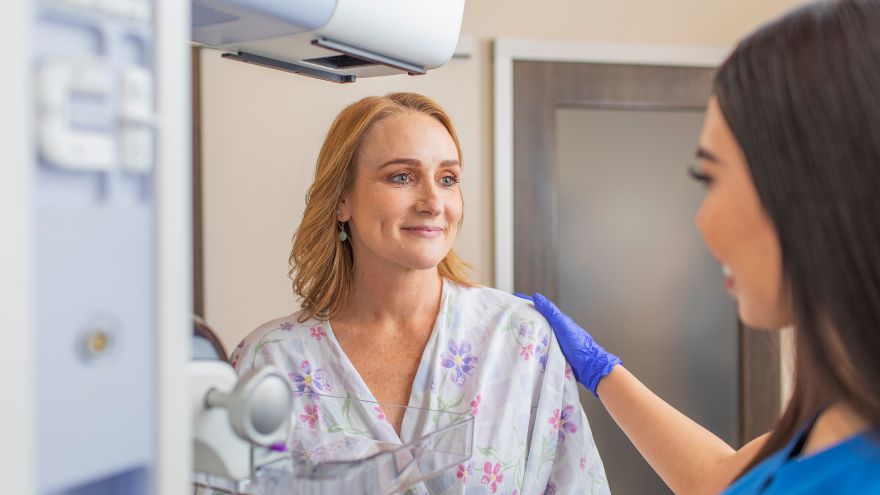
Why Mammograms Are Vital for Early Breast Cancer Detection | Renown Health
Breast cancer affects 1 in 8 women in the U.S. each year, making early detection crucial in improving the chances of successful treatment. Early Detection for Treatment and Peace of Mind Mammograms are noninvasive X-rays used to detect cancer and other abnormalities in the breast. They are the most effective screening tool for detecting breast cancer early, allowing for timely treatment before the disease can spread and helping to improve treatment outcomes. To help guide you through the mammogram process, we spoke with Elizabeth Kang, PA-C, at Renown Breast Surgery Care to equip you with expert knowledge on what to expect and why screening is so important. How Accurate are Mammograms? 3-D mammography technology at Renown Breast Health Center can detect 41% more cancers and reduce the number of false-positive results compared to plain film mammography. Benefits of 3-D mammography include: Providing better, clearer images, with higher diagnostic accuracy Allowing radiologists to see more abnormalities in the breast Helping doctors spot more cancers and avoid false positives, especially if you have dense breast tissue Reduced callback rates for findings on screening Mammogram Screening and Breast Exam Recommendations Renown Women's Health recommends the following breast exam guidelines: Age 18-39: Consult your primary care provider for a Risk Assessment and start breast exams at age 25. Age 40+: Get your annual mammograms. Family history: Begin screening 10 years before your youngest family member's age at diagnosis. For example, start at age 35 if a family member was diagnosed at 45. Self-awareness: Be familiar with the look and feel of your breasts and report any changes to your care provider. Age 75+: Continue annual mammograms if life expectancy exceeds five to seven years. What screenings are available for women with breast implants? Women with breast implants can and should still receive mammograms, and it’s essential to have these screenings done by an experienced team. Be sure to inform your healthcare provider and mammogram technicians about your implants, as they may recommend special techniques or steps to detect abnormalities and ensure accurate results.
Read More About Why Mammograms Are Vital for Early Breast Cancer Detection | Renown Health
-
Department Spotlight: Child Life
March is National Child Life Month. Join us in recognizing our Child Life team at Renown Health! The hospital environment can be a daunting and confusing place for a child. Whether they are admitted to the hospital themselves or have a family member who is currently undergoing treatment, they undoubtedly bring along a lot of overwhelming questions and concerns. No one would be better to guide them through the process than the Child Life department at Renown Health. Our devoted Child Life Specialists and Child Life Assistants dedicate themselves to helping our youngest patients and children of relatives in the hospital cope with their anxieties and fears. With the smiling faces of the Child Life team on their side, children at Renown have a sense of solace while they are in the hospital with a team to cheer them on every step of the way. Offering a Hand to Hold From the first moment of a child’s visit to Renown, they are never alone. The Child Life team, which is made up of three specialists and two assistants, is here to provide a helping hand throughout the entire hospital process, explaining each test, procedure and process every step of the way and creating the best possible plan for each patient – all while fostering and maintaining a safe and supportive environment. “We are specifically trained to help patients and families throughout their healthcare experiences,” said Amanda Cleary, MS, CCLS, Child Life Specialist. “This looks different for every family. We are trained to tailor our services to meet individual family and cultural needs based on our assessment.” “It does not take long for a Child Life Specialist to create a safe relationship with a pediatric patient,” added Angie McEvers, CCLS, CFLE, Child Life Specialist. “The Child Life department can help any care team do their job by redirecting a child’s focus and distracting them from painful interventions, and this is a win-win for both the patient and the care team.” This team’s primary goal is to make talking to doctors and undergoing tests a little less intimidating for our youngest patients. Interaction is a crucial part of a child’s healthcare journey. Our Child Life Specialists are masters at procedure preparation, surgery preparation, trauma support and diagnosis education while meeting each child where they are at developmentally. “A day in the life of a Child Life Specialist is never the same, and every child is different,” said Jennifer Nunzir, CCLS, Child Life Specialist. “To make sure patient care is possible, I make sure I am here mentally for the patients and families. I am ready with a smile to greet them and try to make them comfortable from the start. We are always present to support a patient and family with a new diagnosis, talk to children when there has been a tragic accident, make memories for families and giving children a distraction from tests and procedures.” “One of the biggest benefits to our job is our ability to provide emotional support and communicate with families in a way that makes them feel seen and heard,” added Amanda Cleary. “We listen to the family’s past medical experiences and work on building rapport by building those connections. When you get a child to open up, you see who they are as an individual, and we build from there.” The efforts of the Child Life team go beyond helping children with coping skills. They also jump in with activities to keep kids of all ages engaged – from arts and crafts to pet therapy. “Bringing children smiles through play and giving them fun things to do – whether it’s watching a movie, playing a game, doing an art project, going for a wagon ride or taking them to the Children’s Healing Garden – makes me feel I am making a difference,” said Jennifer Nunzir. “If I can get the child and family to at least smile or laugh, I feel I have already eased some fear and anxiety. It truly is the best feeling to get them smiling and laughing.” “Through play, conversation, distraction or relaxation techniques, patients cope better, and families are calmer,” added Angie McEvers. Teaching Every Step of the Way Education is a crucial aspect in this department. Each Child Life team member works closely with their patient’s care teams to break down “doctor speak” with age-appropriate explanations. “Children come into the hospital for all sorts of reasons, from a broken bone to cancer; our background in child development and psychology helps us collaborate with the patients’ providers and explaining what each part of the care journey is depending on a child’s developmental level,” said Amanda Cleary. “For example, we can explain what a brain tumor is with playdough and help a child with a new diabetes diagnosis understand what it means to balance sugars using play food. It's all about providing family-centered support so that they feel more in control. I can’t tell you how many times I’ve seen parents’ eyes light up when the kids play. They are all coping, learning and growing together.” To Help with the Happy and the Sad When healthcare journeys don’t go as planned, support from care teams is crucial for families facing grief or loss. The Child Life Specialists are one of the first on the scene to provide support for children and their families, providing education on how to talk to children about death and helping families preserve the memories of their loved ones for years to come. “One of the most difficult things we do is provide bereavement support,” said Angie McEvers. “Not only do we provide support for families of pediatric patients but also adult patients who have children. Our team takes the time to help families with memory making with handprints, journals, books, the list goes on. No one should have to go through this process alone, and we make sure that doesn’t happen.” Above all else, the Child Life team are here, first and foremost, for the patients and their families. They are the drive that keeps them going – and helps them reinvigorate that passion for their work every day. “I have met some of the most amazing children and families, and they definitely are what keep me here at Renown,” said Jennifer Nunzir. The Road to Child Life The journey to becoming a Child Life Specialist looks different for every team member, and many of them discovered the field while pursuing careers in other healthcare areas. Beyond their passion for children and families – and their Certified Child Life Specialist credential – our Child Life team members are also highly educated in the fields of human development, nursing and psychology, knowledge that benefits them greatly in their career. Amanda Cleary had the unique experience of pursuing a Child Life career at Children’s Hospital of Los Angeles before she arrived at Renown last year, implementing her knowledge from her bachelor’s degree in human development and family studies into a clinical child life internship and a robust career in Child Life. “While at Penn State, I learned about the Child Life career path through the Children’s Miracle Network Dance Marathon,” said Amanda. “I knew that this was the path I wanted to take. I did a 600-hour internship, and from there I was hired at Children’s Hospital of Los Angeles, where I stayed for 11 years. As a lifelong learner, I knew I wanted to pursue more – so I achieved my master’s degree online in child life leadership and advocacy at the Erickson Institute in Chicago, and what I learned in that program continues to serve me well in my career at Renown.” Other Child Life Specialists, like Angie McEvers and Jennifer Nunzir, had already been with Renown for several years in other departments and built up a wealth of healthcare knowledge before discovering their passion for the mission of Renown’s Child Life program. “I have been here for 23 years; I always knew I wanted to work with children in the hospital because I love kids, and although I originally wanted to be a nurse, I realized that I actually wanted to be on the other side of helping,” said Jennifer. “At the time, I didn’t know there was a job like the Child Life Specialist out there, and I feel so lucky to have found this career. Over the years, as Reno has grown, so has our program, which is very exciting. I knew Renown would be the place where I could grow as well." “This year is my 24th year with Renown,” added Angie. “Before I worked here, I was an Advanced EMT/Firefighter while pursuing my nursing degree. In working with the medical team from Children's Hospital of Oakland in pediatric hematology/oncology, I was able to see first-hand the benefit of Child Life. I was driven to finish my human development degree and passed my certification testing, and ever since then, I’ve been with Pediatrics, PICU and the Children’s ER.” We could not have said it better ourselves – this is a field that is constantly evolving and progressing, and while not everyone is familiar with it, our Child Life Specialists are ready to change that narrative. “There is a lot of opportunity here to continue to grow the Child Life program,” said Amanda. “Not all hospitals have a Child Life program, but we are lucky that Renown does. Any aspiring Child Life Specialist should consider coming here, as it has been a great experience. It is a familial feeling here, and I definitely feel like I am in the right place.” There is Strength in Numbers It takes a village to serve the emotional needs of the many children and families that walk through the doors of Renown Children’s Hospital, and our Child Life Specialists are considered some of the key leaders of that village. The outpouring of support for our Child Life program is astonishing. Not only have our patients and employees made generous donations, but members of the greater Reno-Sparks community are always there ensure kids in the hospital can be kids. The Nevada Wolf Pack, SCHEELS, Great Reno Balloon Race and Atlantis Casino are just a few of the many generous organizations that have donated both toys and time to our youngest patients. To support any child dealing with a serious illness, especially cancer, Beads of Courage steps in to help children “visually record, tell and own their stories of courage” using beads as a symbol. Representatives from Beads of Courage volunteer their time to help our youngest patients keep track of their valiant fight against their illness, adding a bead to their necklaces after every step in their care journey. “We rely on our generous community and donations that come in, and we see a lot during the holiday season – we definitely can benefit from this year-round,” said Amanda. The donations allow the Child Life team to expand their play, coping and distraction opportunities for patients and families, allowing them to reach more children within their small, mighty and growing team of five. “Our goal as a team is to work with as many pediatric patients and children of relatives seeking treatment as possible, so the opportunity to grow our team would be awesome,” said Amanda. And grow they will! The team recently welcomed two dedicated Child Life Assistants, Marissa Arriaga and Sydnee Patterson, during Child Life Month. These team members work alongside the Child Life Specialists to help provide opportunities for developmental play, both in the playroom and at the bedside. Marissa and Sydnee ensure that the kids can still be kids, even while they are in the hospital. Additionally, the Child Life department is currently hiring more Child Life Specialists. If this line of work speaks to you or someone you care about, they are strongly encouraged to apply, because in the end: "We do it all for the kids,” closes Jennifer Nunzir.